Table of Contents
- What are heart valve diseases?
- How is heart valve replacement surgery performed?
- Kalp kapağı tedavisinde ameliyatsız yöntemler var mı?
- Is a biological valve better or a mechanical valve?
- How many years do heart valve replacement patients live?
- What happens if I don't have heart valve surgery?
- Is heart valve surgery risky?
- When is heart valve surgery performed?
- References
What are heart valve diseases?
KProblems with alpine lids generally occur in two types: Either there is a problem opening the valve or there is a problem closing it. If there is a problem with opening, there is a valve stenosis (e.g; aortic valve stenosis, mitral valve stenosis); valve insufficiency if there is a problem with closure (e.g; aortic valve insufficiency, mitral valve insufficiency) takes its name. Sometimes, stenosis and leakage coexist in the same valve.
Note In colloquial language, the word “valve” is often used instead of “valve”; the two are synonymous. Similarly, the words “insufficiency”, ”insufficiency“ or ”leakage" also mean the same thing.
The valve problem can be mild, moderate or severe. Mild or moderate problems do not cause any complaints and do not require intervention; therefore, it is sufficient for the patient to remain under medical supervision. ProvinceIf there is a severe problem, i.e. severe valvular stenosis or regurgitation, it is usually athe appendix is intervened. The intervention is either valve surgery or non-surgical. With surgery, cover replaced or repaired. In non-surgical methods, interventions on the valve are performed without cutting the rib cage and without stopping the heart. Which treatment is suitable for which patient varies from patient to patient.
Let's take a brief look at heart valve replacement surgery, heart valve repair surgery and non-surgical methods.
How is heart valve replacement surgery performed?
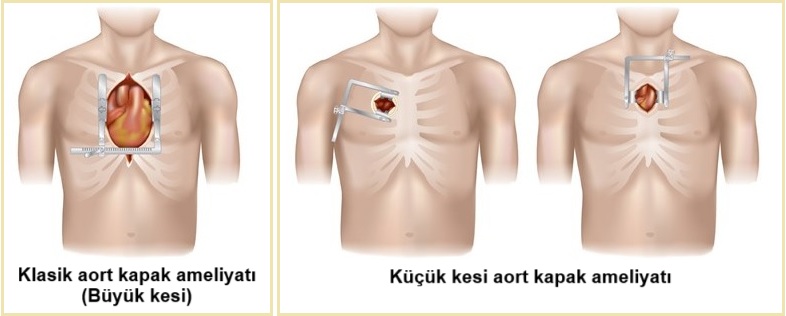
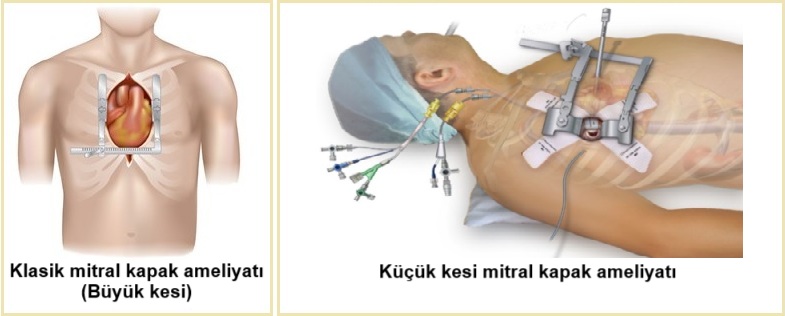
In heart valve replacement surgery, the patient is first connected to a ventilator and put to sleep under general anesthesia. The chest cage is opened by cutting the skin, subcutaneous tissues and the breastbone. The heart is stopped. When the heart is not functioning, the heart-lung pump is responsible for pumping and oxygenating the blood. Then, the left atrium for the mitral valve and the aorta for the aortic valve are cut and the valve is accessed. The old valve is cut out and the new artificial valve is sewn in place. At the end of the operation, the patient is weaned off the heart-lung pump and the chest is closed with metal wires. This one, classical surgery method.
What is closed heart valve surgery?
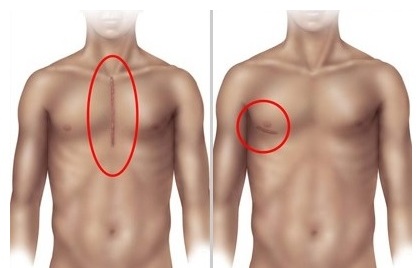
Thanks to advances in technologyNew methods have been developed as an alternative to the classic surgery described above. For example, the operation can be performed through a small incision in the side of the chest. Minimally invasive method In this method, both valve replacement and repair can be performed. Popularly known as “closed surgery” or “surgery with small incision” known as “open” surgery. In fact, this is also a type of "open" surgery. Another method is to perform the surgery using a robot (Robotic surgery). In this method, several small holes are made in the chest through which the rods of the robot are inserted into the chest. The surgeon does not touch the patient directly; he or she performs the operation by controlling the robot's arms from a corner of the operating room. These alternative methods allow for a shorter recovery time and a smaller aesthetic scar. However, the surgeon who performs them must be a physician who has been trained in these techniques and has sufficient experience.
What is heart valve repair surgery?
When surgery is needed for heart valves (especially, mitral and tricuspid valve) If the valve anatomy is appropriate and the surgeon has sufficient experience, valve repair is preferred over valve replacement. This is because, in case of repair, the patient will have his/her own natural valve after surgery and will not have to use strong blood thinners for the rest of his/her life. However, this is not always possible. In this case, the valve must be replaced. Different methods can be applied for repair. For example, if the threads holding the valve are broken, they can be replaced with artificial threads, if the natural ring that holds the valve is enlarged, it can be contracted with bracelet-like materials, or if there is extra tissue in the valve structure, it can be cut out.
Video 1. Aortic valve surgery (AVR)
In recent years, thanks to advances in technology, it has become possible to treat heart diseases with non-surgical methods as an alternative to surgery. The reason why these methods are called "non-surgical" is that, unlike surgery, the chest cage is not cut and the heart is not stopped during this treatment. In other words, all the steps are done while the heart is still functioning. Because the heart is not stopped and therefore does not need to be connected to a heart-lung pump, the risks of these procedures are generally lower than with surgery. Because there is no incision in the chest, the healing process is faster. Pain and stress are also less. There are no aesthetic problems as there are no scars on the chest. Usually through the groinThis is done with the help of long, flexible tubes (catheters), which are inserted into the heart through a small vascular access that is thinner than a pencil. The most typical example is the non-surgical replacement of the aortic valve of the heart (TAVI). A similar method is used for the pulmonary valve of the heart. For the other two valves of the heart (mitral and tricuspid valves), this method is not yet suitable due to anatomical difficulties. However, studies are ongoing and it is expected that these valves will also be replaced without surgery within 10 years. Nevertheless, in today's modern medicine, mitral valve stenosis in appropriate patients balloon expandable (mitral balloon) or mitral valve leakage latch method (MitraClip / Pascal) can be partially or completely corrected by the method. All these non-surgical methods are performed by interventional cardiologists (surgeries are performed by cardiac surgeons).

Prof. Dr. Şükrü Akyüz is an interventional cardiologist. His specialty is the treatment of heart diseases with non-surgical methods. He is a proctor (trainer) and consultant for structural heart disease procedures, including the latch method and TAVI.
Is a biological valve better or a mechanical valve?
There are two types of artificial valves: Biological (tissue) valve and mechanical valve. Which patient is better suited for a biological valve and which patient is better suited for a mechanical valve is evaluated individually for each patient, as each has its own advantages and disadvantages.
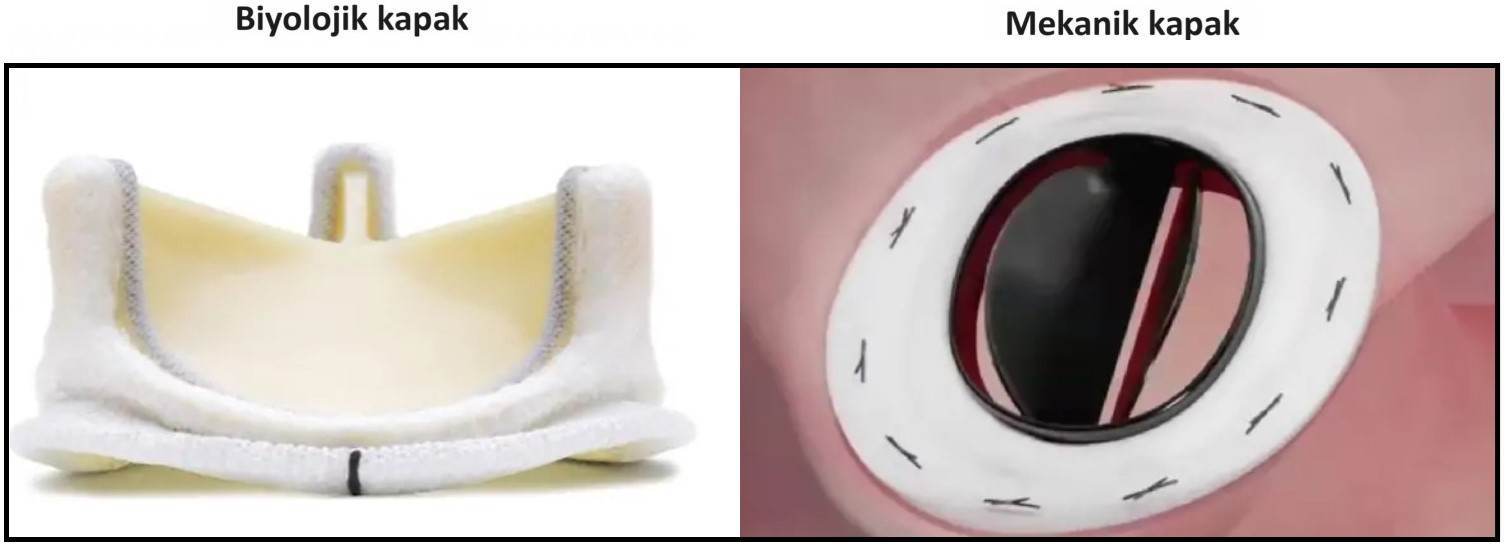
- Biological cover, It is made from the heart membrane of cattle or pigs and looks like a natural valve. It fails earlier than a mechanical valve. In particular, it deteriorates even earlier in relatively young people (due to the fact that the heart of young people works harder and the blood passing through more quickly tires and strains the valve more). For this reason, the biological valve is preferred in older people, taking into account the patient's expected natural life expectancy.
- Mechanical cover, It is usually made of carbon and metal and works like a hinge. It is preferred in younger people because it does not deteriorate easily. However, since this valve is not biological, the body tries to form a clot much more strongly against this valve, which it sees as a foreign substance. If a clot develops, the valve hinges may become blocked and stop working. Therefore, mfor the mechanical cover a powerful drug called warfarin blood thinners must be taken for life (according to the most up-to-date information, no other blood thinners can replace warfarin). This medicine is laborious to use. It increases the tendency to bleed, it interacts with certain foods and medicines (i.e. its effect is either increased or decreased), especially green leafy plants, and its effectiveness (i.e. how “diluted” the blood is) needs to be checked every month with a blood test (INR). With a biological valve, a milder blood thinner such as aspirin, which is easier to use, is sufficient, and so the problems seen with warfarin are usually not seen.
Note In non-surgical methods (e.g. TAVI), only a biological valve can be implanted, not a mechanical valve, because the mechanical valve is inflexible and cannot be compressed into the catheter. Also, ga woman planning to become a midwife, a biological valve is usually preferred. This is because the blood thinner warfarin, which has to be used with a mechanical valve, has the potential to damage the development of the fetus and lead to a malformed birth.
How many years do heart valve replacement patients live?
It is not possible for a doctor to know exactly how long a patient in relatively good general condition will live. In his experience, he can only make an estimate for patients who are in a very serious condition, or, based on statistics, he may be able to estimate the life expectancy of similar patients for a certain period of time. average can give life expectancy. To summarize, to give a general idea:
- Since mitral valve surgery is riskier than aortic valve surgery, the life expectancy is shorter.
- People with a weak heart pump have a shorter life expectancy than those with a normal heart pump.
- Those with serious problems in other vital organs (brain, lungs, liver or kidneys) live less long than those without.
- Not surprisingly, those who have surgery when they are older live less long than those who have surgery when they are younger.
- Most importantly, those who have surgery too late live less than those who have surgery on time.
The newest and most comprehensive scientific research on life expectancy is on aortic valve replacement (Surgery and TAVI) (See. References). Accordingly, for those who had surgery before the age of 50, life expectancy is about 4 years shorter than the average life expectancy of healthy people. After the age of 80, the life expectancy for those who had surgery is almost the same as that of their healthy peers.
If the surgery is performed promptly and with a good surgical technique, and if the patient takes good care of himself/herself, that is, if he/she takes his/her medication regularly and follows a healthy lifestyle such as eating and walking, the chances of living a normal or near-normal life are quite high. For example, a recent and comprehensive study on survival after repair surgery for degenerative mitral valve disease concluded that: “If mitral valve repair is performed by experienced surgeons and on time, these patients live as long as healthy people” (See. References).
Our experience is that the mitral valve modified the results of the patients' mitral valve repair not as good as the ones that have been done, but we do not have sufficient and reliable data to quantify this.
What happens if I don't have heart valve surgery?
The heart when the valves are severely stenotic or leaky, It cannot do its job properly; it cannot send enough blood and therefore oxygen to the body. In order to compensate for this, the heart has to work harder and over time it becomes tired and the pumping power of the heart decreases, i.e. heart failure develops. Although this time varies from patient to patient, eventually severe shortness of breath due to heart failure reaches an incurable stage and the patient dies.
Is heart valve surgery risky?
Heart valve surgery is a major operation and carries serious risks, such as stroke and death. Of course there is. However, the risk of surgery should be compared to the question "What is the risk if I do not have surgery?". For risk, there are risk tables or software created based on scientific data. The risk is calculated by entering the patient's data. Examples of these data that affect the risk are as follows: The age of the patient (especially, the level of indulgence in the general condition of the patient, i.e. his biological age), concomitant diseases of other organs (Alzheimer's disease, chronic renal failure, cirrhosis, COPD, etc.), low pumping power of the heart, concomitant cardiovascular disease (i.e. a combination of valve and bypass surgery), etc. Let's not forget: Fearing these risks and not undergoing surgery will result in the onset of a grueling process without treatment and ultimately death for most patients. For example, let's say the risk is calculated as %5. That is, for every 100 patients who undergo surgery, only 5 will not survive the operation or will develop another serious complication such as paralysis, or, in reverse, 95 will successfully complete the operation. In this case, someone who refuses to undergo surgery because they are afraid of the %5 probability described by the doctor, maybe not immediately, but eventually result kesin olan seçeneği (%100 ölüm) tercih etmiş olur. Not having surgery in time and having surgery when the disease has progressed further requires a more risky operation than a few years ago, as the heart's pumping power has been greatly reduced. Sometimes the risk of surgery is really high, but a non-surgical solution is possible. In this case, it is better to opt for less risky non-surgical methods (TAVI, MitraClip, etc.). Sometimes the disease is so advanced that neither surgery nor non-surgical methods can provide a solution. In this process, called palliative treatment, the focus is on treatments that allow the patient to breathe as comfortably as possible for the rest of his/her life, rather than correcting the disease.
When is heart valve surgery performed?
New onset of symptoms (signs or symptoms) is an indication that the disease has progressed and it is time for surgery. For example, symptoms such as shortness of breath, chest pain or palpitations when walking or climbing hills are important. However, it should be kept in mind that these symptoms can also be caused by another disease such as anemia or COPD. The time of onset of symptoms is different for each patient. In some patients, symptoms appear relatively early in the course of the disease, while in others, symptoms occur when the disease is very advanced. In other words, serious problems may have started in the heart before the symptoms appear and it may be time for surgery. For this reason, the patient should be followed up regularly with various tests, especially echo (heart ultrasound). In these follow-ups, the enlargement of the heart chambers or a decrease in the pumping power of the heart indicates that it is time for surgery, even if the patient has no complaints.
References
- Otto CM, Nishimura RA, Bonow RO, et al. ACC/AHA Guideline for the management of patients with valvular heart disease. J Am Coll Cardiol. 2021 Feb 2;77(4):e25-e197.
- Vahanian A, Beyersdorf F, Praz F, et al. ESC/EACTS Guidelines for the management of valvular heart disease. Eur Heart J. 2022;43(7):561-632.
- Otto CM. Timing of aortic valve surgery. Heart. 2000;84(2):211-218.
- Glaser N, Persson M, Jackson V, et al. Loss in life expectancy after surgical aortic valve replacement. Swedeheart study. J Am Coll Cardiol. 2019 Jul 9; 74(1):26-33.
- Watt TMF, Brescia AA, Murray SL, et al. Degenerative mitral valve repair restores life expectancy. Ann Thorac Surg. 2020 Mar;109(3):794-801.
- Attinger-Toller A, Ferrari E, Tueller D, et al. Age-related outcomes after transcatheter aortic valve replacement: insights from the SwissTAVI registry. JACC Cardiovasc Interv 2021;14:952-960.

