Table of Contents
- What is coronary artery disease?
- What are the symptoms of coronary artery disease?
- What does the percentage of stenosis in a vessel mean?
- How is vascular stenosis different from vascular occlusion?
- Why does coronary artery disease happen; what are the risk factors?
- How is coronary artery disease diagnosed?
- What are the complications of coronary artery disease?
- How is coronary artery disease treated?
- How should people with cardiovascular disease eat?
- Can vascular stenosis regress?
- Stent or bypass?
- References
What is coronary artery disease?
The heart cannot use the blood in its cavities directly. Like other organs, it receives oxygen through its own vessels. The first vessels that branch off from the aorta, which distributes the blood pumped by the heart throughout the body, also belong to the heart and run on the outside of the heart. In medicine, they are called “coronary arteries”. There are two main arteries in the heart: The right main artery and the left main artery. The left main artery is called the LMCA and the right main artery is called the RCA. The LMCA is a short but wide artery that divides into two branches: LAD and CX. Because each of these two branches is as large as the right main artery, they are also sometimes called the main arteries. For this reason, in everyday life, one might also say “there are three main arteries in total, two on the left and one on the right”.
Some people have fatty deposits on the walls of blood vessels that gradually build up over the years. If these deposits (plaque) become too large, the space through which the blood passes narrows. This means that the inner surface of the heart vessels becomes more or less protruding. This is called “coronary artery disease”. Coronary artery disease is synonymous with “cardiovascular disease”. It is also known colloquially as “arteriosclerosis” and “cardiovascular occlusion”.
How many types of coronary artery disease are there?
There are two main types of coronary artery disease:
Kronic coronary syndrome: Over the years, the intravascular space gradually narrows. One day it no longer allows enough blood to pass through and the patient begins to complain. The most common complaint is chest pain when walking but not at rest, or a feeling of discomfort in the chest. Patients should note that their symptoms do not start suddenly, but have been present for weeks or months. (chronic) that they exist. A common synonym is "sstable coronary artery disease".
Acute coronary syndrome: This form is sudden; that is, it covers emergency situations. Heart attack types fall into this group. The most common type of heart attack is as follows: The plaque in the coronary arteries suddenly ruptures and the clot, which was intended to repair the rupture, suddenly (acutely) blocks the artery and inadvertently blocks the blood flow to the heart.
What are the symptoms of coronary artery disease?
The signs (symptoms) of coronary artery disease vary from person to person, depending on the severity of the disease. Some people have no symptoms at all. Some people may have mild episodes of chest pain when moving (exercising), while others may have very severe chest pain even at rest. Symptoms may not be noticeable at first or may only occur when the heart beats very fast, such as when playing sports. As the stenosis progresses, less and less blood reaches the heart tissues and the symptoms become more severe and more frequent.
Chest pain is the most common symptom of coronary artery disease. Some people confuse it with heartburn or indigestion. It can feel like pressure, burning or tightness in the chest. Some patients describe it not as pain but as a feeling of unease. They may say, “It feels like someone is sitting on my chest” or “I feel like they are squeezing my chest with a vice”. Chest pain usually occurs in the center or left side of the chest. Exercise or stress can trigger symptoms. The pain usually disappears a few minutes after the triggering event has ended. In some people, the pain may be short or sharp and felt in the neck, arm or back. In some patients, there is no pain at all and the feeling of shortness of breath is more pronounced.
What is angina?
When chest pain is caused by the heart tissues not getting enough oxygen, it is called "angina". So angina is a special type of chest pain.
What does the percentage of stenosis in a vessel mean?
Genellikle, damar çapının %40’a kadar daralması sorun yaratmaz, geri kalan %60 açıklıktan yeterince kan geçer. Darlık %70’den fazla olduğunda ise hemen her zaman kan akımı azalır. Ara yüzdedeki darlıklarda (%40-70) ise kan akımı kişiden kişiye farklılık gösterir; kiminde yeterlidir, kiminde yetersiz. Bu durumda, kan akımının azalıp azalmadığı MPS (sintigrafi), IVUS (damar içi ultrason) ya da FFR denilen tetkiklerle ölçülüp netleştirilir.
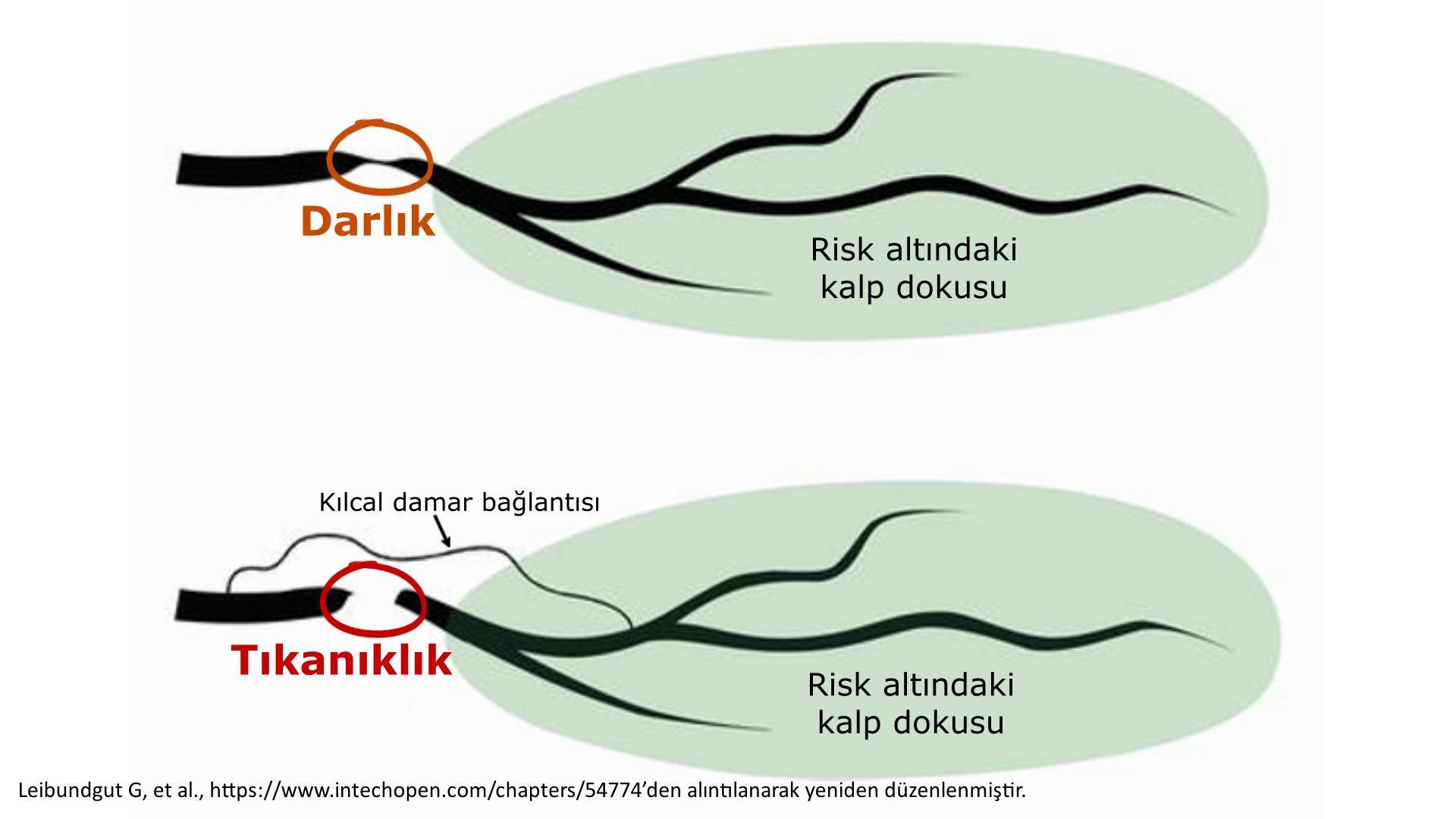
How is vascular stenosis different from vascular occlusion?
If there is a stenosis in a blood vessel, there is still a small opening in the vessel through which blood can pass, even if only a little. In a blockage, the vessel completely closed. Thanks to the small opening in the case of stenosis and the capillary connection in the case of obstruction, the affected heart tissue can receive enough oxygen to survive, although it cannot function fully. The blockage can be soft or hard. The blockage in a heart attack is caused by a clot and is therefore soft. For vessels that have been blocked for more than 3 months, chronic complete occlusion (CTO: Chronic Total Occlusion) the expression is used. CTOs are quite tough.
Why does coronary artery disease happen; what are the risk factors?
- Age: The frequency of coronary artery disease increases with age. The arteries also age.
- Gender: Men are generally at higher risk of coronary artery disease. However, the risk also increases in women after menopause. However, the accuracy of this information is not clear.
- Family history: Genetics is important in coronary artery disease. In particular, the risk increases if a mother, father or sibling has cardiovascular disease. This is called "family history".
- Cigarette: Even passive inhalation of cigarette smoke increases the risk.
- Hypertension Uncontrolled hypertension increases the risk by hardening the arteries.
- Diabetes (diabetes): It increases the risk both through the direct effect of high blood sugar and indirectly by triggering many risk factors.
- Yühigh cholesterol Too high levels of bad cholesterol (LDL) or too low levels of good cholesterol (HDL) in the blood accelerate the accumulation of fat in the vessel wall. High triglyceride levels also increase the risk, although not as much as LDL.
- Irregular Sleep Sleeping too little or too much increases the risk.
- Alcohol: It used to be thought that drinking small amounts of alcohol, especially wine, could be good for the heart. However, new scientific evidence suggests that it is probably best not to drink alcohol at all. This is the recommendation of the latest (2021) European Society of Cardiology "Guidelines on Cardiovascular Disease Prevention".
- Unhealthy diet: In particular, foods containing trans fats, salt and sugar increase the risk.
- Obesity
- Sedentary lifestyle
- Chronic stress
- Chronic renal failure
- Autoimmune diseases
- High homocysteine level
How does stress damage the heart?
The changes that happen in our body when we are stressed normally protect us from the harmful effects of stress. But this is basically an acquired trait for momentary stresses in nature. If the stress persists, it is counterproductive. The hormone cortisol, which is released in stress, raises blood sugar, cholesterol and blood pressure if it remains high in the blood for a long time. Stressed people also tend to smoke more to combat stress. All these are risk factors for vascular stenosis. Stress also directly impairs the functioning of the vascular wall, making it easier for fat to accumulate and clots to form.
How is coronary artery disease diagnosed?
- ECG (Electrocardiography): This test measures the electrical activity of the heart. Your doctor may order this test to find out if you are having a heart attack or if there are any signs of blocked arteries. It also shows heart rhythm problems.
- Effort test (treadmill): If the symptoms do not occur at rest, but in exertional situations such as walking or climbing hills, your doctor may ask you to do a stress test. During this test, ECG electrodes are attached to your chest and the electrical activity of the heart is monitored during exercise. Today it is not used as often as it used to be. This is because it is wrong in almost one in five people. That is, it can make it look like there is a problem when there isn't, or it can make it look like there isn't a problem when there is.
- Nuclear stress testing [Myocardial perfusion scintigraphy (MPS)]: This test is similar to a stress test, but in addition to ECG recordings, a film of the heart is also taken. The patient is given a radioactive substance. The images of the heart at rest and during strain (stress) are compared. Damaged areas of the heart or areas with reduced blood flow cannot use the radioactive material very well. This allows problem areas to be located. In summary, it does not directly examine the heart vessels, but indirectly examines the tissues supplied by the vessels.
- ECHO (Ecocardiography Heart ultrasound): It uses sound waves to image the heart. In areas with insufficient blood supply, movement is reduced and EKO can be detected. Sometimes, the patient's heart is accelerated or stressed by exercise or medication and hidden problems that are not present at rest are revealed. This method is called "stress ECHO".
- Virtual angioplasty (CT angiography): A special dye (contrast dye) is injected through the arm vein. When the dye reaches the heart Thanks to X-rays images of the heart are obtained. Heart vessels that would not normally be visible using X-rays alone become visible thanks to the dye and the presence of stenosis is detected. It is a test that shows the vessels "directly", not "indirectly" like previous tests. Today, it is the most recommended test for cardiovascular control. However, it should be remembered that there are situations in which each test can and cannot be performed, and doctors try to order the most appropriate test by taking these into consideration.
- Angiography (Coronary angiography): Long, flexible tubes, or catheters, are inserted into the heart to deliver dye directly into the heart vessels. This allows very clear images to be obtained. It is also called cardiac catheterization. If necessary, it also provides access to treatments such as balloons and stents. It is the reference test in the diagnosis of cardiovascular disease.
What are the complications of coronary artery disease?
The most important complications are:
- Heart attack
- Heart failure
- Heart arrhythmia
- Death
How is coronary artery disease treated?
Anyone with heart problems, whether mild or serious, should first of all adopt a healthy lifestyle. These are summarized in the figure below:

Despite all this; medicines, heart surgery (bypass) or non-surgical vessel opening methods (stents) may be required.
Which medicines are used in coronary artery disease?
Drugs to relieve chest pain and similar symptoms of coronary artery disease either increase blood flow (and therefore oxygen supply) by dilating blood vessels in areas outside the stenosis, including the reserve vessels, or they help to conserve oxygen. To conserve oxygen, they either increase the heart'sprevent unnecessarily fast beats or positively alter intracellular metabolism pathways. As a result, the heart does more work with less oxygen. These medicines include:
- Beta blockers These medicines slow down, or rather normalize, the heart rate. This helps to reduce symptoms such as chest pain. They also help to keep blood pressure under control.
- Calcium channel blockers: These drugs have a similar mechanism of action to beta-blockers.
- Nitrates They work by dilating the heart vessels. Long-acting ones work throughout the day. Short-acting ones in the form of sublingual pills or sprays are used to quickly relieve chest pain.
- Ranolazine: It is a new generation of drugs. The mechanism of action is not clear, but it is likely thatThey have an impact by ensuring the economical use of oxygen.
- Trimetazidine This is also The mechanism of action is not clear, but it is likely thatThey work by ensuring the economical use of oxygen. It is not considered as effective as ranolazine.
Other drugs are aspirin and cholesterol-lowering drugs. However, their intended use is different. Neither has a direct effect on symptoms such as chest pain; their main effect is to reduce the risk of heart attack and death.
- Aspirin: Aspirin is a blood thinner, which means it reduces the tendency of the blood to clot.
- Cholesterol-lowering drugs: Regardless of the cholesterol level, they help to reduce the build-up of fat in the vessel wall that leads to stenosis. The most important of these drugs are statins (atorvastatin, rosuvastatin, pitavastatin, etc.).
How is a stent inserted?
What is bypass surgery?
How should people with cardiovascular disease eat?
Recommended by international guidelines Mediterranean style Remember that this way of eating applies to everyone, whether they have cardiovascular problems or not. The difference in cardiovascular disease is that tighter to comply with the law (See. References).
- Eat a diet based on vegetables and fruits. Make sure they are fresh and in season.
- Eat more nuts such as walnuts, hazelnuts and almonds (unsalted and raw), fish, legumes (dried beans, kidney beans, chickpeas, lentils) and fiber.
- Don't eat too much bread. But, ever It is not right not to eat bread. Choose whole wheat bread instead of white bread.
- Cut down on sweets and sugary drinks (cola, soda, fruit juices, etc.); if possible, eliminate them from your life. Ask for water or mineral water with your meals.
- Avoid processed meats (sausages, pepperoni, salami, etc.). In fact, avoid everything processed.
- Use less salt; no more than 5 grams per day.
- Avoid snacks such as fast food, chips and biscuits.
- Choose low-fat or fat-free dairy products.
- Avoid trans fats such as margarine. Cook with healthier fats such as olive oil or sunflower oil.
- Do not consume too much animal fats (saturated fats) such as butter. In fact, with the new data, this issue has become somewhat controversial. Namely, ever It is probably not right not to consume it. For example, you can eat butter for breakfast. It is also okay to eat eggs.
- You can eat up to 500 grams of lean red meat per week. However, we do not recommend eating offal.
- You can also drink herbal teas, black tea and coffee twice a day, but too much can cause palpitations.
- Although a plant-based diet is generally considered to be healthier, do not be under the misconception that all plant foods are beneficial and all animal foods are harmful. For example, remember that white flour and refined sugar, which are known to be harmful, are plant foods, while fish, which is known to be beneficial, is an animal food.
- “Can veins be opened with herbal treatment?", which we recommend you also read.
Can vascular stenosis regress?
Although lifestyle modification and the use of medication can rarely lead to regression of plaques in the vessel wall, their main benefit is to consolidate the plaques and reduce the likelihood of cracking or, if not regression, at least prevention of rapid progression. In summary, the main goal is to prevent the progression of vascular stenosis, not its regression.
Stent or bypass?
Heart surgeons and interventional cardiologists are two different groups of doctors who treat problems with blood vessels. Cardiac surgeons solve vascular problems with surgery (bypass), while interventional cardiologists solve the same problems with non-surgical methods (complex stenting procedures). For this important topic, see the related, detailed our article we recommend you to read it.

Prof. Dr. Şükrü Akyüz is an interventional cardiologist. His professional interest is the treatment of heart diseases with non-surgical methods. This includes the non-surgical opening of complex vascular blockages with special stenting methods.
References
- Virani SS, Newby LK, Arnold SV, et al. AHA/ACC/ACCP/ASPC/NLA/PCNA Guideline for the management of patients with chronic coronary disease. Circulation. 2023 Aug 29;148(9):e9-e119.
- Vrints C, Andreotti F, Koskinas KC, et al. ESC Guidelines for the management of chronic coronary syndromes. Eur Heart J. 2024 Sep 29;45(36):3415-3537.
- Byrne RA, Rossello X, Coughlan JJ, et al. ESC Guidelines for the management of acute coronary syndromes. Eur Heart J. 2023 Oct 12;44(38):3720-3826.
- Rao, S, O'Donoghue, M, Ruel, M. et al. ACC/AHA/ACEP/NAEMSP/SCAI Guideline for the management of patients with acute coronary syndromes. JACC. 2025;85 (22):2135-2237.
- Visseren FLJ, Mach F, Smulders YM, et al. ESC Guidelines on cardiovascular disease prevention in clinical practice. Eur Heart J. 2021 Sep 7;42(34):3227-3337.
- Arnett DK, Blumenthal RS, Albert MA, et al. ACC/AHA Guideline on the primary prevention of cardiovascular disease. Circulation. 2019 Sep 10;140(11):e596-e646.

