Table of Contents
- STENT OR BYPASS?
- RECOMMENDATIONS FOR PATIENTS AND RELATIVES
- FREQUENTLY ASKED QUESTIONS
- How long does a stent and bypass take?
- Can't I be treated with medication instead of a stent or bypass?
- What are the risks of stents and bypass?
- Is a stent or bypass better for the left main artery (LMCA)?
- If there is a blockage in all three main vessels, is a stent or bypass better?
- What is the hybrid method?
- Can a medicated balloon save a patient from a stent or bypass?
- How many years will a patient with a stent live?
- How many years does a bypass patient live?
- EXAMPLES OF OUR COMPLEX STENT CASES
- REFERENCES
STENT OR BYPASS?
Is a stent or a bypass better for treating a blocked heart artery? This is a common question and the answer is different for every patient. Because everyone is different. Doctors take many factors into account before making this decision and decide what is best for you. In this article, I will summarize the general principles that should be considered when making this decision.
Note In order to better evaluate this article “Stent“ and “Bypass Surgery“ I suggest you read the articles I wrote about it.
Unfortunately, the information you hear from your friends, read on the internet, see on social media, or watch on TV morning shows about how heart disease is treated may not be up-to-date and accurate. My personal experience is that the information on these platforms is often outdated and scientifically incorrect. Therefore, when making a treatment decision about a vital organ such as your heart, you should make sure that the information you hear has scientific references and that the doctor providing the information actually has up-to-date theoretical knowledge and clinical experience in the relevant field. Ultimately, the best decision for you will be made by a doctor who understands your medical condition and is up to date with the latest scientific data.
Cardiac surgery and cardiology are two different branches of medicine that treat heart diseases. While cardiac surgeons solve problems in the heart through surgery (bypass); interventional cardiologists solve the same problems with non-surgical methods (stent). Both stenting and bypass surgery, heart vessel blockagesof are effective methods of opening up. Let's elaborate on this a little bit, but first, let's talk briefly about what a stent and bypass are:
Stent, and the blockages in the blood vessels is a tubular scaffold used for trenching. Bypass surgery is a type of surgery that restores blood flow by connecting additional vessels beyond the blocked areas of the heart vessels. In some patients, stenting is the only option and bypass is inappropriate or unnecessary. In some patients, the opposite is true, i.e. bypass is the only option and stenting is inappropriate or unnecessary. In this patient group, cardiologists and cardiac surgeons usually they are in agreement. But what do you do if one doctor recommends a stent procedure and another doctor recommends bypass surgery? You will naturally be confused here. In fact, in most patients, both are preferable; eitherni neither is wrong. This may seem counter-intuitive: “When it comes to human health, how can the right approach not be clear?” But it is current scientific data, in appropriate patients shows that both treatments are correct. Objective; klynical and anatomical both methods To explain the scientific pros and cons of both methods to a suitable patient in a way that they can easily understand and to ensure that the patient takes an active role in the final decision.
When explaining why he or she recommends a stent or bypass, your doctor will tell you about The severity of your heart disease, additional problems in other organs and your general health.
- The severity of your heart disease: In the left main artery (LMCA: Left main coronary artery) straits, fully occluded vessels (CTO: Chronic total occlusion) or blockages in multiple vessels means that the condition is “complex”, i.e. difficult and complicated. These are the main reasons why a patient is offered bypass surgery.
- Additional problems with your other organs: The risk of bypass surgery increases if you also have serious problems with vital organs such as the lungs, liver, kidneys and brain. For example, if the condition of the vessels on angiography suggests that bypass would be a better option, but you also have a serious lung disease such as COPD, a stent is now a better choice than a bypass because of the possibility of not being able to leave the ventilator during surgery. Conversely, even if you are initially thought to have a vascular problem that can be solved with a stent, if you are also found to have a problem with your heart valves and this problem can only be solved with heart valve surgery, then bypass may be preferred; thus, both your vascular and valve problems can be solved with a single operation.
- Your general state of health: Some patients cannot even go to the toilet in daily life without help, i.e. they are very debilitated. These patients may not be able to tolerate bypass surgery and a stent may be preferred over a bypass.
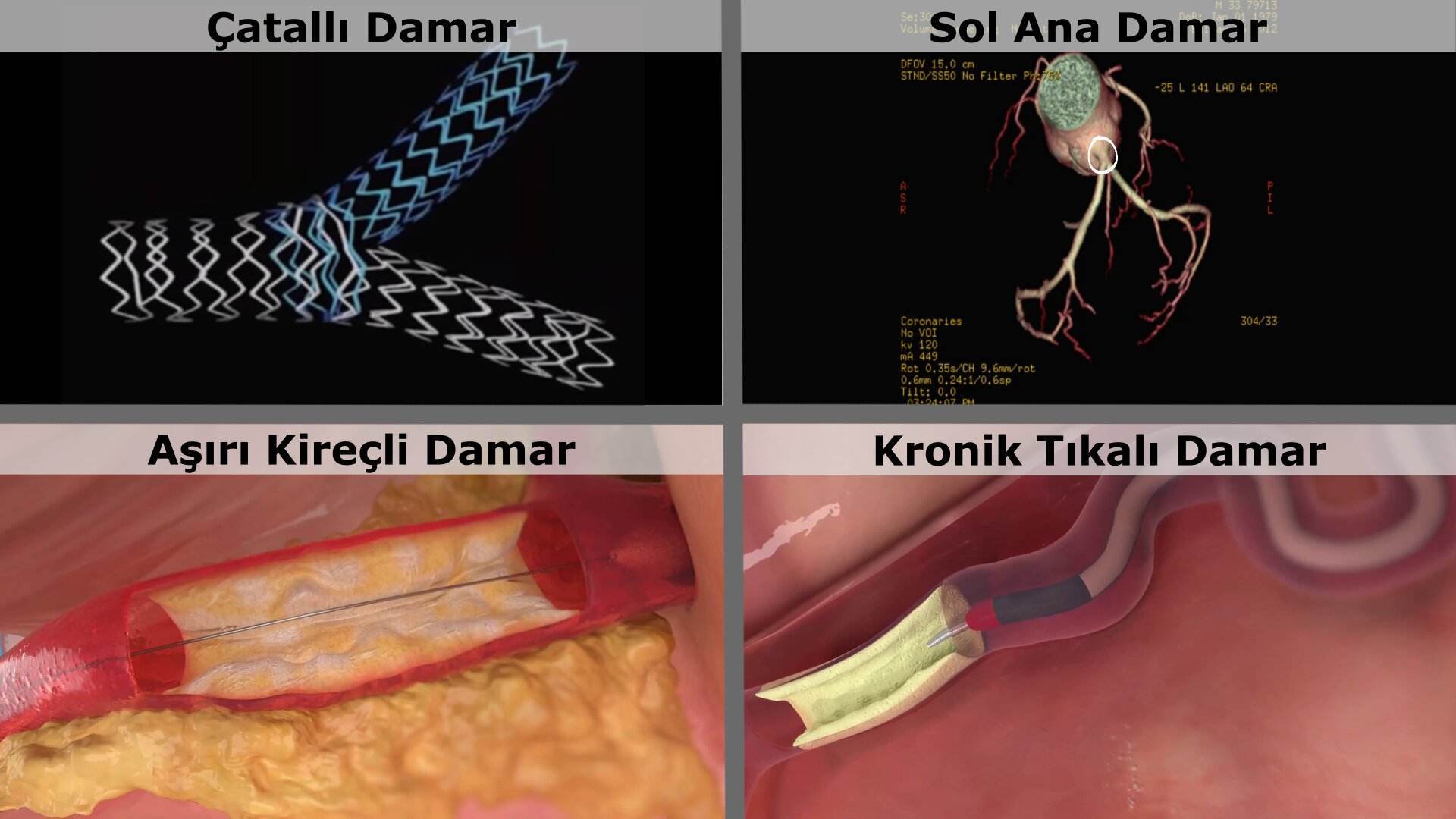

Thanks to advances in technology, today, an experienced interventional cardiologist whose professional interest is in complex procedures can open complex blockages in the arteries with a stent instead of bypass surgery. The stent provides the same benefit in most patients in whom bypass surgery is decided. That is, in these patients, bypass surgery and stenting are equally effective; neither is wrong. However, some patients still require bypass surgery (see References).
RECOMMENDATIONS FOR PATIENTS AND RELATIVES
- If you consulted a cardiac surgeon, more bypass; if you consulted an interventional cardiologistif you have applied more in favor of the stent. This is a natural human reflex and usually neither is wrong.
- For complex cases to be solved by stenting, it must be within the interventional cardiologist's professional interest. Not every cardiologist prefers to deal with complex cases, nor is it an obligation. First of all, complex stenting procedures require years of training.
- Having bypass surgery for the second time is quite risky. Stents are generally preferred in these patients.
- In patients with a narrowed or blocked stent, the problem can be solved by inserting another stent into the stent. In most patients, the stent will not narrow again. However, in rare cases, the stent may narrow again (for the second time). In this case, a stent is usually no longer recommended; drug treatment or bypass is preferred.
- With conventional bypass, a large scar remains on the leg and chest where the vessel was removed. The legs may also develop permanent edema (swelling). If this is a major aesthetic concern for you, opt for alternative (modern) surgery (small incision or robotic bypass) or a stent. The benefit to the heart (e.g. life expectancy) of a small incision or robotic bypass is the same as that of a conventional bypass. The main benefits of these new methods are a better aesthetic appearance and faster recovery due to the absence of large incisions.
- Drug eluting stents are better than non-medicated stents. The latest generation of drug eluting stents are also generally better than the previous generation of drug eluting stents. However, most of the drug eluting stents produced in recent years do not have a significant difference in quality.
- If possible, it is recommended that the veins taken for the bypass should be arteries and not veins (legs). This increases the likelihood that the vessels (grafts) will remain open for many years. For example, if clinically and anatomically appropriate, it is better to use both the left (LIMA) and right thoracic artery (RIMA) than to use only the left thoracic artery and use the leg vein (saphenous vein) for the remaining vessels.
- Bypass usually does not prevent stenting if necessary in the future. Stent placement does not usually prevent a bypass later on either.
- After bypass surgery, the patient is hospitalized for a few days, some of them in the intensive care unit. After stenting, the patient is usually discharged the next day. Patient recovery takes a few weeks for bypass and a few days for stenting.
- Either complex stenting or bypass surgery should be preferred for LMCA or multiple main vessel occlusions. In these cases, simply applying a medicated balloon, as shared on some websites or Instagram accounts, is a procedure whose efficacy and safety have not yet been proven, and its recommendation is medically incorrect.
- Some people cannot overcome their fears and do not want to have a bypass. Therefore, your character and psychological state are important in the choice of treatment.

For serious decisions, such as the choice of treatment, we recommend that you seek a second opinion from a different physician. It is important that you request that the most up-to-date scientific evidence for the proposed treatment is presented in understandable language, with references.

Prof. Dr. Şükrü Akyüz is an interventional cardiologist. His professional interest is the treatment of heart diseases with non-surgical methods. Among these treatments is the non-surgical opening of complex vascular blockages with special stenting methods.
FREQUENTLY ASKED QUESTIONS
How long does a stent and bypass take?
The duration of the stent procedure depends on the anatomical features of the vessels and how many vessels will be stented. In complex cases it is usually 1.5-2 hours. Bypass surgery, gIt usually takes 3-4 hours. The time required depends on the type of bypass surgery (classic, small incision, etc.) and how many vessels will be bypassed.
Can't I be treated with medication instead of a stent or bypass?
In many, but not all, cases, medication is actually preferable to stenting. Nowadays, medications that allow the heart to use oxygen sparingly or to dilate the heart vessels to deliver more blood flow and oxygen can provide similar benefits without stenting. The biggest benefit of the stent is that it relieves the patient's symptoms faster than medication (usually from the next day) and reduces the number of medications to be used over a lifetime. A stent can be used in some special cases (e.g. LMCA stenoses, blockages at the beginning of the left anterior main artery or blockages in more than one main artery).) prolongs the patient's life, while emergency stenting in cases such as heart attacks saves lives. BIn these special cases, medication alone is not as helpful as a stent. Surgery is a treatment method that is mostly used in these special cases. If vascular problems are serious enough to warrant surgery, medication alone is insufficient.
What are the risks of stents and bypass?
Like any other procedure, both stenting and bypass surgery have risks. The risk actually varies from person to person. For example, emergency procedures during a heart attack are riskier. Procedures performed on patients with other serious diseases are riskier, even if they are performed by the most experienced physicians. Complex cases are also riskier. Common complications that can occur with both procedures include the following:
- Vascular damage: Mild bruising at the insertion site is normal in stenting. Severe bleeding or blockage of the groin or wrist vein may occur. Therefore, blood transfusion or emergency vascular surgery is rarely necessary. Similar problems can occur in the neck and other vascular access points for the administration of medication, blood and fluids during surgery.
- Arrhythmia Short-term rhythm disturbances of the heart that go away on their own are common, but usually of no significance. Rarely, emergencies requiring medication or electric shock can occur.
- Kidney failure: The dye (contrast medium) that allows us to obtain images during the stenting procedure impairs the kidneys in 5 out of every 100 patients on average. The risk is even higher in patients who already have kidney problems. For example, the risk is 5 times higher in advanced kidney failure. The kidney impairment that develops is usually temporary; it resolves completely with intravenous fluid replacement. Very rarely, temporary dialysis may be needed. Kidney failure can also occur during surgery, when the heart is stopped and the heart-lung pump is switched to a heart-lung pump, so that the kidney receives less blood.
- Allergy Allergy may rarely develop due to the dye used in the stent procedure. Itchy rashes may occur on the skin, but these are temporary. Very rarely allergic reactions are serious enough to prevent breathing. Drugs given for general anesthesia during surgery can also cause allergic problems.
- Heart attack In stenting, if the patient's vessels are very fragile, the catheters can damage them. It is usually not possible to recognize this risk in advance. This can rarely cause a heart attack and the patient may need urgent heart surgery. If the operation takes a long time, part of the heart may lose its vitality after the operation and permanent damage (heart failure) may occur. In rare cases, both the stents and the vessels (grafts) in the bypass can become blocked and cause a heart attack.
- Paralysis Small fats or clots that break off when the catheter touches the delicate areas of the vessels that allow us to access the heart can escape into the brain vessels; temporary or permanent paralysis (stroke) can develop. Strokes can also occur during surgery due to fat in the vessel (aorta) to which the heart-lung pump is connected or clots that form in the system.
- Rupture, tear or puncture of a heart vessel: These problems rarely develop with stenting. In most cases, the problem is solved with emergency interventions during the procedure. Very rarely, a needle may need to be inserted into the chest to drain the blood collected in the pericardium or emergency surgery may be required. In bypass, there may also be blood leakage from the places where the vessels are stitched and the patient may need to have his or her chest opened again.
- Death: Emergency interventions may not work and in rare cases the patient may die.
- Other: In addition to surgery, the following can happen: Infections of the skin, subcutaneous tissue, bone or deep areas of the chest where the incision was made (mediastinitis), pneumonia, lung collapse (atelectasis), clots from the leg to the lungs (pulmonary embolism), inflammation of the lining of the heart (acute pericarditis or Dressler's syndrome), hardening of the lining of the heart and compression of the heart (constrictive pericarditis), memory loss and difficulty thinking clearly.
Is a stent or bypass better for the left main artery (LMCA)?
LMCA stenosis is a more serious problem than any other vascular stenosis. This is because the LMCA is the largest heart vessel. In the past, LMCA stenoses required bypass surgery; there was no other solution. Now, an experienced interventional cardiologist can alternatively open this vessel - including the area where it is bifurcated - with a non-surgical method, i.e. stenting. However, the choice between surgery and non-operation is determined by the degree of complexity of the blockage. For this, the angiogram is monitored and calculated. Syntax score is important. According to the recommendations of the ESC (European Society of Cardiology) guidelines, which are based on scientific data, in most cases of LMCA (Syntax score <33), a stent provides similar long-term benefit to bypass surgery. In LMCA patients with additional complex stenoses in other major vessels (Syntax score ≥33%), bypass surgery is preferred. However, Syntax score ≥Even if it is 33%, if surgery is too risky for the patient and therefore the patient or the surgeon is not considering surgery, then stenting is better than just managing with medication.
The following is a joint publication of the ESC (European Society of Cardiology) and EACTS (European Association for Thoracic, Cardiovascular and Thoracic Surgery) in 2023 “LMCA (Syntax score <33) Consensus Report“between the two methods. This figure is designed to help patients better understand the results between the two procedures. As you can see from this figure, 84 out of every 100 patients do not develop any problems with the bypass and 80 out of every 100 do not develop any problems with the stent over 5 years. So, the difference is 4 per 100 patients. Ultimately, the patient evaluates the significance of the %4 event difference in this comparison from their own perspective and has the right to make the final choice based on the pros and cons between stenting and bypass surgery. After all, the body is the patient's body and it is the duty of doctors to respect the patient's choice (See. References).
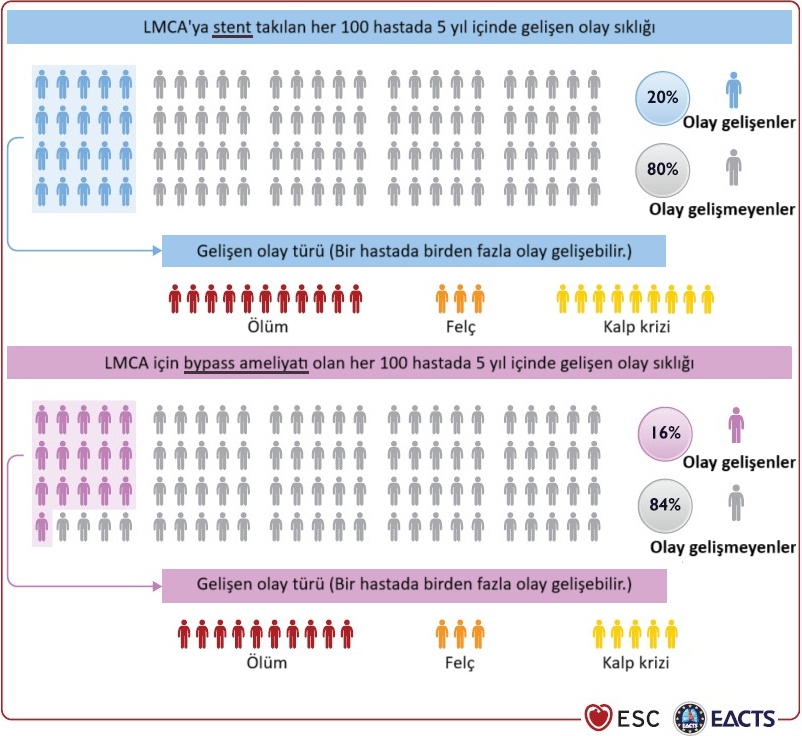
If there is a blockage in all three main vessels, is a stent or bypass better?
In the past, patients with stenosis in all three main arteries (LAD, CX, RCA) had no choice but bypass surgery. Similar to the LMCA, there have been improvements here over the years. Unless very complex (Syntax score <33), these vessels can now be opened with a stent without surgery. However, this information is only valid for non-diabetics. Because in diabetics with triple-vessel occlusion, bypass surgery is relatively more effective on survival and is still the preferred method.
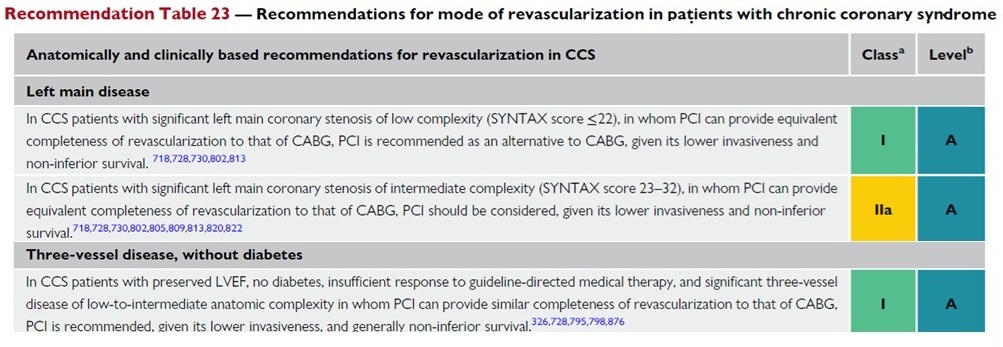


Turkish translation of the table above:
2024 ESC Chronic Cardiovascular Disease Treatment Guidelines
A report prepared by the European Society of Cardiology (ESC) working group Approved by the European Association for Cardiovascular Surgery (EACTS).
Table 23 - Recommendations for the choice of vascularization methods in chronic cardiovascular disease
Left main:
- In the treatment of patients with mildly complex left main stenosis (Syntax score ≤22), stenting is recommended as an alternative to bypass surgery if all stenoses can be opened with a stent as well as with bypass surgery. This is because in this case, the intervention is milder with a stent and the patient's life expectancy is as good as that of bypass surgery (Class IA).
- In the treatment of patients with moderately complex left main stenosis (Syntax score: 23-32), stenting should be considered as a treatment option if all stenoses can be opened with a stent in a manner equivalent to bypass surgery. Because, in this case, the intervention to the patient is milder with stenting and the patient's life expectancy benefits as much as bypass surgery (Class IIA).
Tri-vascular disease (No diabetes):
- In the treatment of patients with severe stenosis in all three main vessels, mild or moderately complex anatomically, but who are not diabetic, stenting is recommended if there is no response to medication in accordance with the guidelines, if the heart's pumping power is normal, and if all stenoses can be opened with a stent equivalent to bypass surgery. This is because in this case, the intervention is milder with a stent and the patient's life expectancy is usually as good as that of bypass surgery (Class IA).
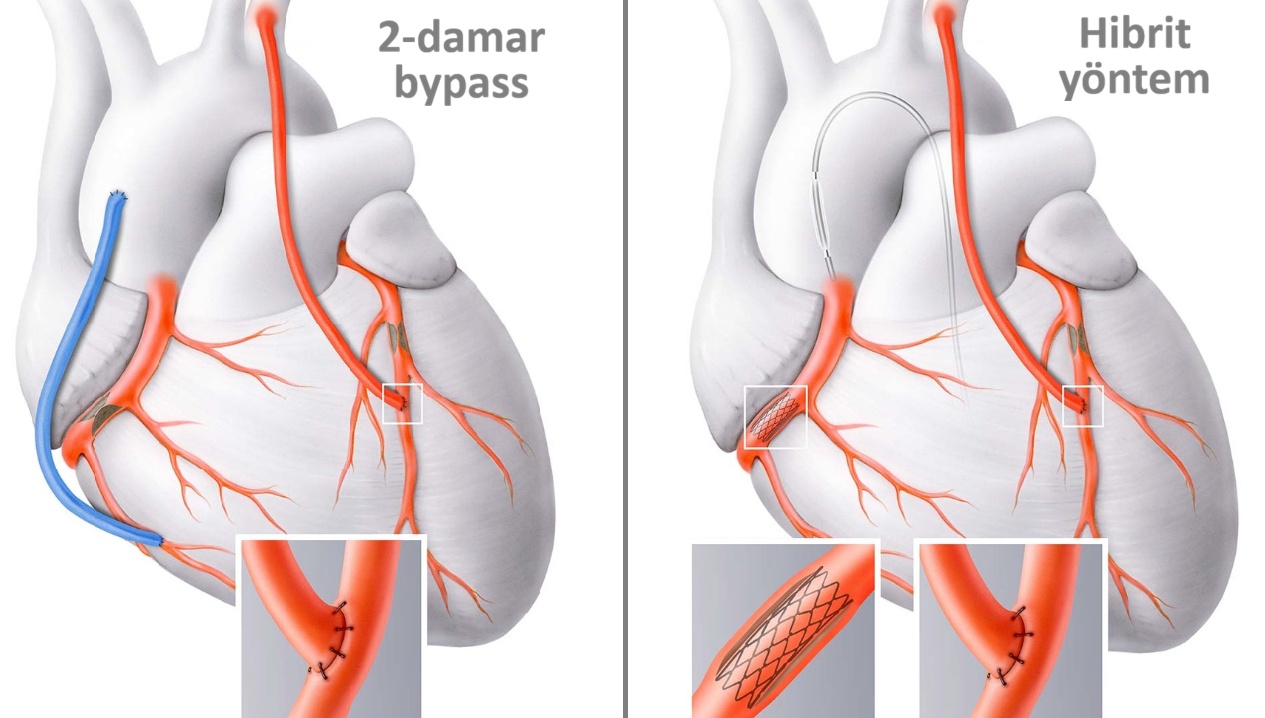
What is the hybrid method?
Sometimes, there are cases where stenting and bypass surgery alone are not the solution; you have to combine them in a planned way. Let's present an example case:
A 68-year-old patient with chronic renal failure has a left anterior main artery (LAD) stenosis that is not suitable for stenting because it is too long and has ballooned (aneurysmatic) areas. In addition, there are stenoses in the left lateral main artery (CX) and the right main artery (RCA). However, bypassing these vessels is not appropriate. This is because a graft cannot be taken from the leg because of severe leg vascular disease and from the right arm because of a dialysis fistula. Moreover, it is not easy to sew these grafts to the aorta because of the calcified (porcelain) aorta. In this case, the most appropriate method would be to perform bypass surgery on the LAD and then stent the RCA and CX. This way, all vessels are opened in the best way and the risk is reduced as the operation time is shorter. Apart from this example, there are many other situations where the hybrid method may be preferred.
Can a medicated balloon save a patient from a stent or bypass?
LMCA veya 3 ana damar tıkanıklıklarında güncel bilimsel kılavuzlar bypass ameliyatı veya kompleks stentleme önermektedir. Bu damarları ilaçlı balonlar da genellikle açar; ama, mevzu sadece “damarı açmak” değildir. Evet, damar balonla kısmen bile olsa açıldığında (örneğin; %90 darlık, %50’ye gerilediğinde) kan akımı artacağı için hastanın şikayetleri ilk başta geçer. Ama, “Will the vein stay open in the long run?” The question is much more important. Unfortunately, however, it is not uncommon for some social media accounts and websites to claim that the medicated balloon can open the vessels without even stenting, i.e. without leaving any metal behind, thus saving patients from complex stenting or bypass surgery. This is contrary to scientific guideline recommendations and medically incorrect because it is potentially error-prone. So, are we sure that the fate of medicated ballooning in these cases will not be disappointing in the long term, like the fate of dissolving stents in the past? If future comparative quality scientific studies prove that drug-eluting balloons are as good as drug-eluting stents in complex cases, of course, most interventional cardiologists, myself included, would prefer drug-eluting balloons over drug-eluting stents. Because it is much easier to perform a medicated balloon than a complex stenting procedure. After all, ballooning is basically the act of inflating a balloon; it is not as dependent on the physician's knowledge, experience, dexterity and specialized materials as stenting.
For more information about medicated balloons related articlez You can read it here.
Will the stent get blocked?
It is very important that the interventional technique applied during stenting meets the minimum necessary conditions in terms of stent occlusion. After a technically successful stent procedure, the patient's regular use of medications, control of risk factors such as high blood pressure and diabetes, quitting smoking and starting to practice other healthy lifestyle changes will help the stent to prevent excessive tissue growth over time. significantly reduces the likelihood of narrowing or occlusion (in-stent restenosis).
In complex cases, there are usually problems in more places, so more stents are needed. The more and longer the stent, the more likely it is that excessive tissue growth will occur. in the stent stenosis or obstruction the more likely it is to develop. However, this should not be interpreted to mean that the stents are likely to narrow. In 10 years stentte development of stenosis; in only 1 in 10 uncomplicated cases while the complex one occurs in 2 out of 10 cases. Tersten okunduğunda, kompleks olmayan vakaların %90’ında, kompleks vakaların ise %80’inde stentlerde darlık gelişmez. If a problem develops, in most cases it happens within the first year. Also, For those who develop stenosis, a second procedure solves the problem in about half of the cases and stenosis does not develop again. Therefore, stents do not have a certain lifespan; it varies from person to person.
Stent with clot suddenly blockage leading to a heart attack, adevelopment of stenosis in the stent due to excessive tissue growth It is a different issue and occurs in only 1 out of every 100 people. Although there are many reasons for this, the most common reason is that the patient is not taking his/her blood thinners. Blood thinning medicinesafter the tent is installed not to use it, especially in the first months, is life-threatening.
Are bypass vessels blocked?
Unlike a stent in bypass surgery of the inserted veins (graft) the likelihood of narrowing or blockage gradually increases over the years. In 1 in 10 cases, the grafts become occluded within 1 month. This is often due to technical inadequacy. The likelihood of blockage depends on the type of graft. Aarterial grafts (from the chest and arm) are used in only 1 in 10 people. In 10 years tıkanır. Tersten okunduğunda, atardamar olan greftler %90 vakada en az 10 yıl boyunca çalışır. Oysa, toplardamar olan greftler (bacaktan alınanlar) her 10 kişiden 5’inde 10 yıl içinde tıkanır; hatta bu tıkanma vakalarının yarısı bunu ilk 1 yıl içinde yaşar. That is, the use of arteries provides the best results in terms of vascular patency in the long term. To summarize, of the grafts. does not have a definite lifespan; çin most patients grafts with arteries remain open for life (See. References).
How many years will a patient with a stent live?
It is not possible to know exactly how many years the patient will live. Estimated percentages can only be given by looking at the statistics of previous patients with the same characteristics. The most important factors that negatively affect this statistic are the following: Technical inadequacy in the stenting procedure, holder age, heart failure, heart valve disease, the presence of serious diseases in other organs, hypertension, diabetes, high cholesterol, smoking, medication non-compliance and lack of social support.
How many years does a bypass patient live?
After bypass surgery, most patients feel better and have no complaints for many years. However, over time, the newly inserted vessels can become blocked and stent or a second bypass surgery may be required. It is difficult to predict how many years the patient will live. In some patients (e.g. cases with serious problems in one of the other vital organs) can be as short as a few years, while in some patients life expectancy is the same as in healthy people. Similar to patients with stents, the above factors that affect statistics also play a role in patients with bypass.
EXAMPLES OF OUR COMPLEX STENT CASES
CASE 1
- Issue: In the anterior main artery of the heart (LAD) curved there's a shortage in the area.
- The decision at another hospital: Bypass surgery.
- Patient's decision: The patient, who was informed in detail, did not want to undergo surgery due to anxiety.
- Final decision: Opening the vessel with complex stenting techniques.
- Interventional cardiologist Prof. Dr. Şükrü Akyüz
- Conclusion: Successful.
CASE 2
- Issue: In the main vessels of the heart, two different forked there are bottlenecks in the region.
- The decision at another hospital: Bypass surgery.
- Patient's decision: The patient, who was informed in detail, did not want to undergo surgery due to anxiety.
- Final decision: Opening the vessel with complex stenting techniques.
- Interventional cardiologist Prof. Dr. Şükrü Akyüz
- Conclusion: Successful.
CASE 3
- Issue: The left main artery of the heart (LMCA) there's a stenosis in the risk zone where it bifurcates.
- The decision at another hospital: Since the patient also had serious problems in his lung and kidney, bypass surgery would be very risky, so risky stenting was performed with the decision of the committee.
- Patient's decision: He approves stenting, even if it is risky.
- Final decision: Opening the vessel with complex stenting techniques.
- Interventional cardiologist Prof. Dr. Şükrü Akyüz
- Conclusion: Successful.
CASE 4
- Issue: Located in the main vein (CX) on the side of the heart stent completely blocked (CTO: completely blocked vessel).
- The decision at another hospital: Medical follow-up, i.e. a medication solution.
- Patient's decision: He confirms that he will use the medicines appropriately.
- Final decision: Although this decision was initially appropriate, the patient's chest pain when walking persisted despite multiple medications. The final decision was therefore to open the chronic complete occlusion with complex stenting techniques. Bypass surgery for this side vein is already not among the options.
- Interventional cardiologist Prof. Dr. Şükrü Akyüz
- Conclusion: Successful.
CASE 5
- Issue: The anterior main artery of the heart (LAD) is divided into two forked both stenosis and CTO (completely occluded vessel).
- Patient's decision: The anatomy is suitable for both surgery and stent. The patient, who is informed in detail, prefers the stent.
- Decision: Opening the vessel with complex stenting techniques.
- Interventional cardiologist Prof. Dr. Şükrü Akyüz
- Conclusion: Successful.
REFERENCES
- Vrints C, Andreotti F, Koskinas KC, et al. ESC Guidelines for the management of chronic coronary syndromes. Eur Heart J. 2024 Sep 29;45(36):3415-3537.
- Lawton JS, Tamis-Holland JE, Bangalore S, et al. ACC/AHA/SCAI Guideline for coronary artery revascularization. J Am Coll Cardiol. 2022;79:e21-e129.
- Stefanini GG, Alfonso F, Barbato E, et al. Management of myocardial revascularization failure: An expert consensus document of the EAPCI. EuroIntervention. 2020 Dec 4;16(11):e875-e890.
- Byrne RA, Rossello X, Coughlan JJ, et al. ESC Guidelines for the management of acute coronary syndromes. Eur Heart J. 2023 Oct 12;44(38):3720-3826.
- Rao, S, O'Donoghue, M, Ruel, M. et al. ACC/AHA/ACEP/NAEMSP/SCAI Guideline for the management of patients with acute coronary syndromes. JACC. 2025;85 (22):2135-2237.
- Byrne RA, Fremes S, Capodanno D, et al. 2022 Joint ESC/EACTS review of the 2018 guideline recommendations on the revascularization of left main coronary artery disease in patients at low surgical risk and anatomy suitable for PCI or CABG. Eur J Cardiothorac Surg 2023 Aug 1;64(2):ezad286.
- Brilakis E. Manual of chronic total occlusion percutaneous coronary interventions: A step-by-step approach, 3rd ed. Philadelphia PA: Elsevier; 2023.
- Brilakis E. Manual of percutaneous coronary interventions: A step-by-step approach, 1st ed. Philadelphia PA: Elsevier; 2021.

