Table of Contents
- What is PFO?
- What is the difference between PFO and ASD?
- How common is PFO?
- What causes PFO?
- What are the symptoms of PFO?
- How is PFO diagnosed?
- PFO nelere sebep olabilir?
- PFO’su olanların dikkat etmesi gerekenler nelerdir?
- Does PFO require treatment?
- PFO kapatma nedir?
- When will I be discharged after the procedure?
- Will the PFO closure device subsequently move?
- Cihaz, vücutta hissedilir mi?
- Cihaz, vücutta ömür boyu kalacak mı?
- PFO kapatma işleminden sonra kan sulandırıcı ilaç kullanılacak mı?
- PFO kapatma vakalarımızdan örnekler
- References
What is PFO?
In the womb, between the right and left atria of the baby's (fetal) heart, there is an opening (hole) through which blood can normally pass. This is a normal part of the fetus' blood circulation. After birth, this hole is no longer needed.in most people it closes by itself. However, in some people it remains open. In medical terms, this hole is called patent foramen ovale (PFO) which means "an oval hole left open".
Halk dilinde PFO için sıklıkla “delik” sözcüğü kullanıldığından yazının devamında kolay anlaşılır olması iChina The word "hole" will be used instead of "opening".
What is the difference between PFO and ASD?
These are both types of hole in the chamber between the atria. However, ASDis a pathological partial failure of the tissue that forms the chamber. The baby is therefore born with a hole in the heart. PFO is not a formation defect, i.e. there is no missing tissue. The presence of a PFO is not considered a disease in itself. For it to be a problem, a clot that has formed elsewhere in the body must also reach the heart. A PFO may be medically important because it allows a clot to pass from the right side of the heart to the left side of the heart, and the clot may travel with the blood to the brain and result in a stroke. However, this probability is extremely low. In other words, unless there is a stroke or some other disease process, the coincidental finding of a PFO in a person has no significance on its own.
How common is PFO?
PFO is quite common; 1 in 4 people have it. This means that sUltimately, this means that 2 billion of the world's 8 billion inhabitants have PFO.
What causes PFO?
It is not clearly known what causes PFO.
What are the symptoms of PFO?
Most people do not have any symptoms or signs that are directly caused by the PFO. PFO is usually detected incidentally during tests for other purposes.
How is PFO diagnosed?
- EKO (Echocardiography; ultrasound of the heart): It is the basic test in the diagnosis of PFO. It is an instrument that works using sound waves. It takes a movie of the heart. The hole and the blood escaping through it can be seen directly. But, in most cases, it cannot actually be seen directly. In this case, "contrast echocardiography" is performed. In contrast echocardiography, water containing bubbles is given through the vein of the arm, these bubbles reach the heart and if PFO is present, it is observed that these bubbles pass from the right side of the heart to the left side.
- TEE (ECHO through the esophagus): ECHO through the esophagus, which is adjacent to the heart, can provide clearer images. To do this, a flexible cable with the diameter of a pencil is inserted into the esophagus. At the end of this cable there is a special mechanism that allows images to be obtained. This allows the size and shape of the opening to be determined in detail. TEE is used to confirm the diagnosis when a PFO is suspected on contrast echocardiography and to guide doctors during non-surgical closure of the PFO.
- Transcranial Doppler: Contrast echo as sIt is an instrument that works by using es waves and water bubbles. However, ultrasound is performed on the skull, not the heart. The aim is to detect water bubbles that pass through the PFO and travel through the blood to the skull (and therefore to the brain). If no water bubbles are detected, the PFO is not present. However, if water bubbles are detected, a TEE should still be performed to confirm the presence of a PFO.
PFO nelere sebep olabilir?
The most important complication of PFO is paralysis (stroke); that is is a blood clot in the brain. Paralysis can be permanent or temporary. The temporary one is called TIA (transient ischemic attack). However, the likelihood of PFO causing a stroke is extremely low (remember, if every person with PFO had a stroke, 1 in 4 people in the world would have a stroke). It is actually the most common cause of stroke, such as clots or bleeding vascular problems. Vascular problems are usually seen in older patients. Therefore, if a young person has a stroke, it is more likely to be caused by a PFO than an elderly person. PFO can very rarely cause complications other than paralysis:
- A clot in the heart vessel (heart attack)
- Clots in organs other than the brain
- Migraine headache
- Air embolism during diving
PFO’su olanların dikkat etmesi gerekenler nelerdir?
- Diving carries a special risk in PFO. However, if the rules of diving are strictly followed, PFO does not prevent diving. However, if the rules are not followed, air bubbles in the vein can pass through the PFO and cause various problems.
- Egzersiz yapmakta sakınca yoktur. Ama, eğer PFO kapatılmışsa ilk 1 ay yarışmalı veya ağır sporlardan kaçınılmalıdır.
- PFO kapatıldıktan sonra şemsiye benzeri cihazın üzerinin dokuyla kaplanması 6 ay kadar sürebilir. Bu süreçte, kana karışan mikroorganizmalar direkt kan yoluyla cihaza bulaşıp infektif endokardit adı verilen ciddi bir enfeksiyona yol açabilirler. Bu nedenle, ilk 6 ay boyunca diş çekimi veya başka bir organdan ameliyat olmak gibi kanamalı operasyonlardan önce antibiyotik alınması gerekir. 6 aydan sonra böyle bir önleme ihtiyaç yoktur. Ama, nadiren, cihazın köşesinden kalıcı kan kaçağı devam edebilir; bu durumda kanamalı operasyonlar öncesinde antibiyotik alınması her zaman önerilir.
- Nikel-titanyum alaşımından yapılmış olan şemsiye benzeri cihazların metalik yapıları gereği emarın (MRI) manyetik alanından etkileneceği zannedilir. Oysa, bu cihazların manyetik alandan etkilenme özellikleri zayıftır; bu nedenle 3 Tesla dahil emar çekilmesinde sakınca yoktur.
Does PFO require treatment?
Most people with PFO do not need treatment. This is because the PFO itself is not considered a disease. For treatment to be necessary, the complications listed above must have developed. BAt this point, the question arises in the minds of many: "I mean, can't we take precautions before we have a stroke? Do we have to wait for a stroke?". However, it is important to remember this: In medicine, treatment decisions are always based on a risk-benefit analysis. The better option is always preferred. For example, if the treatment in question is to close the PFO, the treatment is either to use blood thinners or to close the PFO non-surgically with umbrella-like devices in addition to the medication. However, medication carries the risk of serious bleeding (brain bleeding, stomach bleeding, etc.). Complications such as perforation of the heart may develop in the closure procedure. Therefore, starting these treatments for every patient with a PFO means unnecessarily exposing someone who is extremely unlikely to have a stroke in his/her lifetime to the possible complications of these treatments.
PFO kapatma nedir?
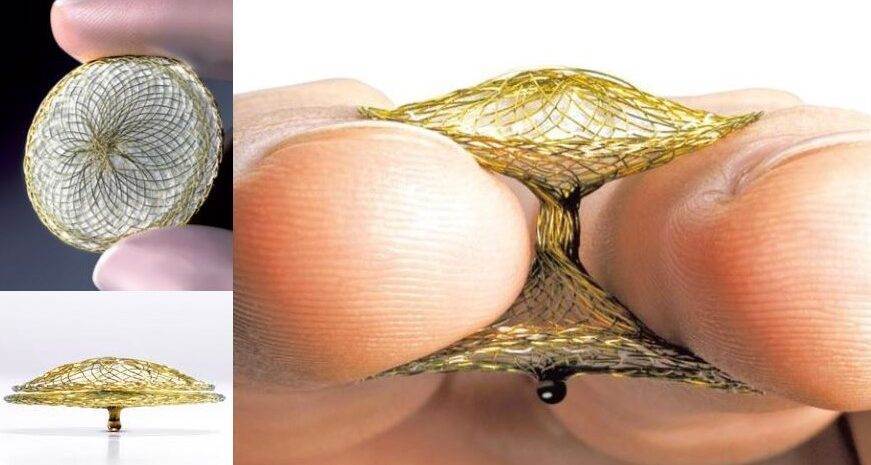
“PFO kapatma” ya da “PFO kapama”, PFO’nun ameliyatsız yöntemle kapatılmasını ifade eder. Bu işlem teknik olarak ASD closure işlemine çok benzer. Girişimsel kardiyologlar tarafından uygulanır. İnce, esnek ve uzun bir boru (kateter) kasık damarı yoluyla kalbe gönderilir. Kateter içinde sıkıştırılmış halde bulunan şemsiye benzeri kapatma cihazı ile PFO kapatılır. Kalp durdurulmadığı ve göğüs kafesi kesilmediği için ameliyatsız yöntem olarak adlandırılır. PFO’yu kapatmak için kalp ameliyatı yapmak tercih edilen bir yöntem değildir. Çünkü, ameliyatsız yöntem çok daha güvenlidir.

Prof. Dr. Şükrü Akyüz, girişimsel kardiyologdur. Uzmanlık alanı, kalp hastalıklarının ameliyatsız yöntemler ile tedavisidir. PFO kapatma da dahil olmak üzere yapısal kalp hastalıkları işlemlerinin proctor (eğitmen) ve konsultanıdır.
When is the PFO closed?
Someone who has had a stroke (temporary or permanent, mild or severe) stenosis in the jugular veink and heart arrhythmia (atrial fibrillation) other causes of stroke are investigated. If the patient does not have any of these causes but has a hole in the heart called PFO, the cause of the stroke is likely to be clots that escape through this hole and travel to the brain. is assumed and the PFO is closed. Bu durumda, tekrar pıhtılaşma olmaması için In addition kan sulandırıcı ilaçlar da (Aspirin, klopidogrel, LMWH veya NOAK’lar…) başlanır.
What is the success rate of PFO closure?
Genel olarak başarı oranı >%95’tir.
What are the risks of PFO closure?
Her girişimsel işlemde olduğu gibi PFO kapatma işleminde de bazı riskler bulunmaktadır. Cihazın yerinden çıkması ve cihaz üzerinde pıhtı oluşması gibi önemli komplikasyonlar her 100 kişiden 1’inde; ölüm ise her 1000 kişiden 1’inde meydana gelir.
Bu riskler nedeniyle endişelenmekte haklı olabilirsiniz; ama unutmayın: Bu komplikasyonlar nadiren gelişirler. Önemli olan, işlemin gerçekten gerekli olup olmadığıdır. Eğer, güncel bilimsel verilere ve kılavuzlara uygun bir şekilde karar verilmişse bu işlemden kaçınmak aslında kendinizi daha önemli risklere (özellikle, felç) çok daha fazla maruz bıraktığınız anlamına gelir.
How long does PFO closure take?
Usually, 1 hour. However, this time may be shorter or longer depending on the anatomical features of the PFO.
Is the procedure performed by stopping the heart, as in heart surgery?
No, it is not. There is no need to stop the heart.
PFO kapatma işleminde ağrı duyulur mu?
No. The procedure is performed either under sedation or under general anesthesia. The difference is that under general anesthesia, a tube is inserted into the patient's respiratory tract and a respirator supplies the patient with air; under sedation, no breathing tube is inserted, the patient is not connected to a respirator, the patient is just put to sleep and breathes on his/her own. In both techniques, the patient is given drugs that prevent the patient from feeling pain during the procedure. General anesthesia (intubation) is more comfortable for the patient.
When will I be discharged after the procedure?
Most patients are discharged the next day.
Will the PFO closure device subsequently move?
Although there are reports in the literature of cases where it appears to have moved afterwards, this is very rare. It is not possible for the device to move after it is covered with tissue within a few months.
Cihaz, vücutta hissedilir mi?
No.
Cihaz, vücutta ömür boyu kalacak mı?
Yes. It is not possible to remove the device back.
PFO kapatma işleminden sonra kan sulandırıcı ilaç kullanılacak mı?
Evet. Genellikle, ilk birkaç ay iki tane kan sulandırıcı ilaç beraber kullanılır; bunlardan biri çoğu vakada düşük doz Aspirin, diğeri ise etken maddesi klopidogrel olan başka bir ilaçtır. Birkaç ay sonra bunlardan biri bırakılır. Sonra, nöroloji hekiminin önerisine göre aynı veya farklı bir kan sulandırıcı ilaç ömür boyu kullanılmaya devam edilir.
PFO kapatma vakalarımızdan örnekler
References
- Kleindorfer DO, Towfighi A, Chaturvedi S, et al. AHA/ASA Guideline for the prevention of stroke in patients with stroke and transient ischemic attack. 2021 Jul;52(7):e364-e467.
- Kavinsky CJ, Szerlip M, Goldsweig AM,et al. SCAI Guidelines for the management of patent foramen ovale. J Soc Cardiovasc Angiogr Interv. 2022 May 19;1(4):100039.
- Pristipino C, Sievert H, D’Ascenzo F, et al; European position paper on the management of patients with patent foramen ovale. Part I – General approach and left circulation thromboembolism. Eur Heart J. 2019 Oct 7;40(38):3182-3195.
- Pristipino C, Germonpré P, Toni D, et al. European position paper on the management of patients with patent foramen ovale. Part II – Decompression sickness, migraine, arterial deoxygenation syndromes and select high-risk clinical conditions. Eur Heart J. 2021 Apr 21;42(16):1545-1553.
- Messé SR, Gronseth GS, Kent DM, et al. Practice advisory update summary: Patent foramen ovale and secondary stroke prevention. Neurology. 2020 May 19;94(20):876-885.

