Table of Contents
- What is a stent?
- Which tests are performed before stenting?
- How is a stent inserted?
- Stent işleminin riskleri nelerdir?
- Stent işleminden sonra ne zaman taburcu olunur?
- Stent takıldıktan sonra fiziksel aktivitelere ne zaman başlanabilir?
- Will the stent move?
- Stent vücutta hissedilir mi?
- Stent, ömür boyu vücutta kalacak mı?
- Stent işleminden sonra kan sulandırıcı ilaç kullanılacak mı?
- Stent yerine ilaçla tedavi olunabilir mi?
- What is the difference between a stent and a balloon?
- What is the difference between a stent and an angioplasty?
- What is the probability of a successful stent procedure?
- One stent at a time?
- How many stents can be implanted in the heart?
- İlaçlı stent nedir?
- El bileğinden mi, kasıktan mı stent takmak daha iyidir?
- What should be considered after a stent procedure?
- Stent kalp krizini önler mi?
- How long does a stent last? Can the stent get blocked?
- How many years will a patient with a stent live?
- Stent or bypass?
- References
What is a stent?
Stent; kalp damar tıkanıklıklarının tedavisinde kullanılan, boru şeklinde bir iskeledir. Krom, kobalt ve platin gibi metallerden yapılır. Angioplasty (coronary angiography), your doctor may recommend that you have a stent. The most common reason for this recommendation is that you have a stenosis or blockage in your heart vessels. The stent procedure helps to keep the vessel open. In many cases, angiography is performed because patients suffer from chest pain. Once the stenosis is opened, the chest pain disappears. Chest pain may have been present for a relatively long time or it may have started suddenly. For this reason, in some people, the stent is inserted in a planned manner, i.e. in non-emergency situations, while in others heart attack gibi acil durumlarda takılır.
Kalp krizi, kalp damarlarının ani bir şekilde often with a clot blockage of a blood vessel. If the vessel is not opened urgently with a stent procedure, heart tissues can begin to die and permanent damage can develop. This can result in heart failure. Heart failure can also develop in non-emergency situations, but it is relatively rare. In this case, the main reason for stenting is to relieve symptoms such as chest pain.

Which tests are performed before stenting?
An ECG is performed before the procedure. Blood tests are also performed to check the risk of bleeding, kidney function and the presence of infection.
How is a stent inserted?
- When you enter the angiography room, you will be asked to lie on a moving table similar to a stretcher. You will be connected to monitors with some cables to monitor your vital functions such as pulse, respiration and blood pressure. On your arm or the back of your hand, as needed Intravenous An IV (intravenous line) will be opened to give fluids and medication.
- The area where the catheter will be inserted (groin or wrist) may need to be shaved just before the procedure. This region, will be wiped with disinfectants to prevent infection. These solutions may be a little cold. Afterwards, your whole body will be covered with a thin sterile dressing.
- Most doctors give you an intravenous sedative to reduce your stress. The area where the catheter will be inserted is then numbed. Within a few minutes, the access catheter (plastic sheath) is placed in your wrist or groin vein. All catheters, wires, balloons, stents, balloons, stents and other devices that will be used during the procedure are sent through this access catheter to the heart. These materials are changed from time to time. During this process, a camera will move around you, sending X-rays and allowing your doctor to take images. This is done to allow better visualization of different parts of the same vessel from different angles. Each time the dye that makes the veins visible is given You may feel a sensation similar to hot flushes; this is a normal feeling and there is no need to worry.
- Most people do not feel any pain during the procedure. Some sensitive people may feel nausea or chest pain due to the effect of the dye injected into the heart vessels or because the balloon inflated to open the vessel temporarily blocks blood flow. However, this is temporary and soon resolves.
- The essential step to open the vessel is to send a hair-thin wire through the stenosis or blockage and beyond the vessel. This wire is used to send a balloon or stent into the problem area. Usually, before stenting, a deflated balloon is first sent into the narrow area and inflated. This allows the relatively thicker stent to pass through the narrow space, determines what diameter stent should be inserted based on the balloon diameter, and sometimes allows additional methods to be applied in advance if a very hardened area due to calcification cannot be opened even with the balloon. Although some patients think that the procedure is performed by "bursting the balloon", the aim is to open the vessel by inflating the balloon without bursting it; in fact, bursting the balloon carries risks and is not something that doctors want, except in some exceptional cases. When the vessel is dilated, the balloon is deflated and removed, but the wire is left in place. In the next step, a stent is inserted to prevent the area of the vessel opened by the balloon from collapsing again, i.e. blocking it. A stent of the appropriate diameter and length is selected to match the diameter and length of the narrow area. The stent is placed on a deflated balloon. When the balloon is inflated, the stent expands and opens, detaches from the balloon and adheres to the vessel wall. The balloon is then withdrawn and the stent is left in the vessel.

How long does the stent procedure take?
Genellikle, 40-60 dk. Ancak, damarın özelliklerine ve kaç damara stent takılacağına göre bu süre değişebilir. Düz damara uygulanan işlem 30 dakikada sonuçlanabilirken, kompleks vakada 3-4 saat sürebilir.
Stent takılırken hasta uyutulur mu?
Only the vein entry site will be numbed so that you do not feel pain. You will be awake during the procedure. However, you may be given relaxing medicines to relieve tension. These may make you slightly drowsy; this is normal.
Stent işleminin riskleri nelerdir?
Her girişimsel işlemde olduğu gibi stent işleminde de bazı riskler bulunmaktadır. Ciddi komplikasyonların her biri her 1000 kişiden 2’sinde gerçekleşir. Risk, aslında kişiden kişiye değişir. Örneğin, kalp krizi sırasında yapılan acil işlemler veya ilaveten başka ciddi bir hastalığı olan hastalara yapılan işlemler en tecrübeli hekimler tarafından yapılsa bile daha risklidir. Kompleks vakaların (sol ana damar, çatallı damar, aşırı kireçli damar veya kronik tıkalı damar -CTO-) işlemleri de daha risklidir.
Olası komplikasyonlar şunlardır:
- Damage to a vein in the leg or wrist: Severe bleeding or blockage of a vein in the leg (groin) or wrist. Therefore, blood transfusions or emergency vascular surgery may rarely be necessary.
- Heart arrhythmia: Short-term rhythm disturbances that resolve spontaneously during the procedure are common but not significant. Rarely, emergencies may occur that impair consciousness and require medication or electroshock.
- Kidney failure: İşlemde görüntü elde etmemizi sağlayan kontrast madde adı verilen boya her 100 hastanın 5’inde böbrekleri bozar. Risk, halihazırda böbrek sorunu olanlarda daha da fazladır. Örneğin, ileri evre böbrek yetersizliğinde risk beş kat daha fazladır. Böbreklerde bozulma gelişse de damardan sıvı takviyesiyle genellikle tamamen düzelir. Bazen, geçici diyaliz gerekebilir. Kalıcı diyaliz gereksinimi ise son derece nadirdir.
- Allergy Allergy to the contrast medium may rarely develop. Itchy rashes on the skin may occur; this is temporary. Very rarely, allergic reactions are serious enough to prevent breathing. All the necessary supplies for such emergencies are available in the angiography room.
- Heart attack Hastanın kalp damarları çok narinse kateter bu damarlara zarar verebilir. Bu, kalp damarlarının tıkanmasına yol açabilir, yani kalp krizine neden olabilir. Bu durumda, damarı açmak için hemen stent takmak gerekir. Çok nadiren, acil kalp ameliyatı (bypass) gerekebilir.
- Heart vessel rupture (dissection) or perforation (rupture): These problems are rare. In most cases, the problem is solved by emergency interventions during the procedure. Very rarely, emergency heart surgery (bypass) may be needed.
- Paralysis Small fats or clots that break off when the catheter touches the delicate areas of the vessels that allow us to access the heart can rarely escape into the brain vessels. This can cause temporary or permanent paralysis.
Due to these risks worrying You may be right, but remember: These complications rarely develop. Önemli olan, stentin gerçekten gerekli olup olmadığıdır. Eğer, güncel bilimsel verilere ve kılavuzlara uygun bir şekilde stent kararı verilmişse bu işlemden kaçınmak aslında kendinizi heart attack means that you may be much more exposed to risks such as death.
Stent işleminden sonra kanama olur mu?
Stent işleminden sonra hemşireniz düzenli olarak kateter giriş yerini (kasık ya da el bileğinizi) kontrol edecektir. Dikkat edilmesi gereken en önemli konulardan biri kanamadır. Kanamayı önlemek için şunlar yapılır:
- If the procedure is performed on the wrist, a bracelet-like, compressive, screw or pneumatic closure device will be placed on your wrist. After 2-3 hours, your nurse will remove it and wrap your wrist with a sterile cloth.
- Vascular access site if the procedure is performed in the groin özel kasık kapatma cihazları ile hemen kapatılabilir. Bu sayede, 1 saat sonra ayağa kalkabilir ve yürüyebilirsiniz. However, if these devices could not be used for reasons such as economic or supply problems before You have to lie on your back for 4-6 hours. At the end of this time, The access catheter will be removed by pulling it out manually and manual pressure will be applied for about 15-20 minutes to control bleeding. Once it is proven that there is no bleeding, you will have to lie flat for an additional 4-6 hours. This means that you will lie on your back for a total of 8-12 hours. During this time, bazı doktorlar kanamayı engellemek için hastanın kasık bölgesi üzerine ağır bir kum torba konulmasını ister. Bunun baskı yaparak kanamayı azalttığı düşünülse de ana mekanizma bu değil; bacağın hareketinin kısıtlanmasını sağlamasıdır. Kişisel olarak ben (Prof. Dr. Şükrü Akyüz), hastanın bacağını oynatmaması gerektiğini anladığından eminsem kum torbası konulmasını tercih etmem. Zaten, güncel tıbbi öneri de artık bu yöndedir. Çünkü, kasık damarından kanama olursa, kanayan bölge kum torbasının altında kaldığı için gözden kaçabilir ve gerekli müdahale gecikebilir. Bunun, hayati risk de dahil ciddi sonuçları olabilir. Ayrıca, kum torbası hastanın konforunu oldukça bozup kötü bir deneyim yaşamasına da neden olmaktadır.
- Yukarıdaki uygulamalara rağmen, nadiren yine de kanama olabilir. Bu durumda, ya kanamayı direkt görürsünüz ya da kasığınızda bir sıcaklık hissedersiniz. Zaman kaybetmeden kanayan yere elle bası uygulamanız ve sonra hemşirenize haber vermeniz oldukça önemlidir.
Stent işleminden sonra ne zaman taburcu olunur?
After the stent procedure, you will be transferred to the coronary intensive care unit or directly to the inpatient ward, depending on the difficulty of the procedure. Often, you will be asked to stay overnight in hospital. Sometimes we may consider discharge on the evening of the day of the procedure, sometimes a few days later. We adjust this according to the complexity of the procedure and your clinical condition.
Stent takıldıktan sonra fiziksel aktivitelere ne zaman başlanabilir?
You should avoid heavy lifting for the first 1 week. The time to drive a car, board an airplane, start work and have sexual intercourse varies according to each patient's condition; you can ask your doctor when you can start these activities. For most people, this is 1 week.
Will the stent move?
No, the stent cannot move, i.e. it cannot slip. If the stent diameter is selected in accordance with the vessel diameter and the stent is found to be stable during the procedure, the stent cannot move afterwards.
Stent vücutta hissedilir mi?
No, it is not. After the procedure, some patients feel a stinging sensation on the left side of the chest and think that it is a stent puncture. However, it is either a psychosomatic pain due to anxiety or pain caused by the stent stretching the vessel wall. These - if any - usually go away within a week.
Stent, ömür boyu vücutta kalacak mı?
Yes. Undoing the stent is out of the question. But it will not do you any harm.
Stent işleminden sonra kan sulandırıcı ilaç kullanılacak mı?
Evet. Stent işleminden önce size başlamış olduğumuz kan sulandırıcı ilaçları you will use it for a few months, sometimes for several years. You will use these periods heart attack the balance between the risk and the risk. After this time, one of the two medicines will be stopped and you will continue with one medicine for life.
Stent işleminden sonra kan sulandırıcı ilaç kullanılmazsa ne olur?
Since the stent is a foreign substance, blood cells (platelets) recognize it and try to cover it with a clot. For this reason, not one but two blood thinners are combined. After a few months, when the stent is covered with enough tissue, the stent is no longer in contact with the blood. Once the stent is embedded in the vessel wall, the risk is reduced, so a single blood thinner is sufficient. Failure to take medication can lead to the stent being blocked by a clot, which can lead to heart attack and can cause sudden death.
Stent yerine ilaçla tedavi olunabilir mi?
Bu soruda, ilaç derken kastettiğimiz göğüs ağrısını kesen ilaçlardır. In many, but not all, cases, medication alone is actually preferable to stenting. Nowadays, similar benefits can be achieved without stenting at all, thanks to medications that allow the heart to use oxygen sparingly or to dilate the heart vessels to deliver more blood flow and oxygen. The biggest benefit of the stent is that it relieves the patient's complaints faster than medication - often as soon as the next day - and reduces the number of medications to be used for life. However, in some special cases medicines stente alternatif değildir. Örneğin, LMCA gibi büyük bir damarı açmak hastanın ömrünü uzatır; bu damardaki sorunlarda ilaçların daha az etkili olduğu kanıtlanmıştır. Kalp krizi gibi acil durumlarda ise stent takmak hayat kurtarır. Aspirin ve statin gibi ilaçlar stent takılsa da takılmasa da zaten kullanılmak zorundadır.
What is the difference between a stent and a balloon?
Both a balloon and a stent are materials used to open a blood vessel. After the balloon, there is a high probability that the vessel will close again. To prevent this from happening, a scaffold is inserted into the vessel. The stent is usually placed. In most cases, the balloon is performed before stent placement to widen the narrowed area of the vessel enough for the stent to pass through and to understand the capacity of the vessel to open. It is also often performed at the very last stage after stent placement to ensure that the stent fits well into the vessel wall and opens properly. The balloon is inflated inside the stent.
What is the difference between a stent and an angioplasty?
Angio does not provide any improvement in the patient. Because there is no intervention in the vessel; the vessel is only visualized. A stent is a device used to open the vessel if a stenosis is detected in the angiogram. In other words, angioplasty one diagnosis method, while stenting is a Treatment method.
In the video below, you can watch two different patients demonstrating the stenting of stenoses in the right and left arteries.
What is the probability of a successful stent procedure?
Genel olarak başarı %90’dan fazladır. Şu durumlarda işlemin başarılı olma olasılığı azalır: Hastanın çok yaşlı olması, tıkanıklığın çok uzun süredir var olması (CTO), kireçli ya da kıvrımlı damar yapısı, kronik böbrek yetersizliği ve yetersiz girişimsel teknik (hekimin tecrübesinin az olması)… Özetle, her hasta için başarı oranı farklıdır.
Stent takma işlemi başarısız olursa hasta daha da kötüleşir mi?
In the event of failure, the condition of your vasculature will usually remain the same. Therefore, your symptoms will not be any worse than before.
One stent at a time?
If there is a problem in more than one vessel or in more than one part of the same vessel, more than one stent can be inserted in the same session. However, if the procedure has taken a long time, we may have to terminate the procedure at that point in order not to increase the possibility that the amount of dye used is too much and your kidney may deteriorate, and in order to prevent both you and us doctors from being exposed to too much radiation. We will complete the missing part at a separate time (session).
How many stents can be implanted in the heart?
Many people think that there is a maximum number of stents that can be implanted in the heart. For example, "No more than 5 stents in the heart" like this. This thinking is wrong. Yes, implanting a large number of stents means that the risks associated with each stent increase. A cardiologist who follows the current scientific data should try to solve the problems with the minimum number of stents that need to be implanted anyway. The main questions to ask here are: "Is it really necessary to implant so many stents?", "Isn't medication enough?", "Bypass surgery is there a better option?". If these questions have been asked and it is decided that one of these methods is actually more appropriate, it would not be right to implant a large number of stents in that patient. However, if it is decided that these options are not clinically appropriate or technically inapplicable, the indication (necessity) is now important, not the number of stents to be implanted. For example, bypass surgery would probably be the best choice for a patient with complex stenoses in many parts of the three main vessels of the heart, who has chest pain even when doing the lightest work and whose pain does not go away despite numerous medications. However, if the same patient has severe pulmonary insufficiency de (e.g. COPD) and is likely to be unable to be weaned off the ventilator after surgery. In this case, the problems in the blood vessels can be solved with a large number of stents.
İlaçlı stent nedir?
İlaçlı stent (DES: Drug-Eluting Stent), metal kısımlarında ilaç içeren stentlerdir. Bu ilaçlar, stentin temas ettiği damar duvarında bulunan damar hücrelerinin çoğalmasını kontrol ederek doku büyümesinin aşırı olmasını engellerler. Böylece, stent içi daralma (ISR: In-stent stenosis) sıklığı azalır. However, stent It is not only whether the stent is medicated or not. The patient's genetic predisposition and technical inadequacies in stent placement can also cause it.
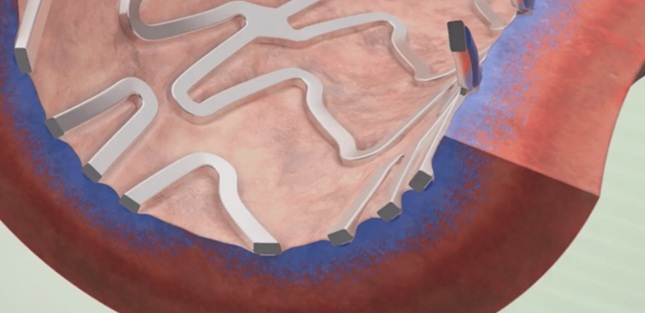
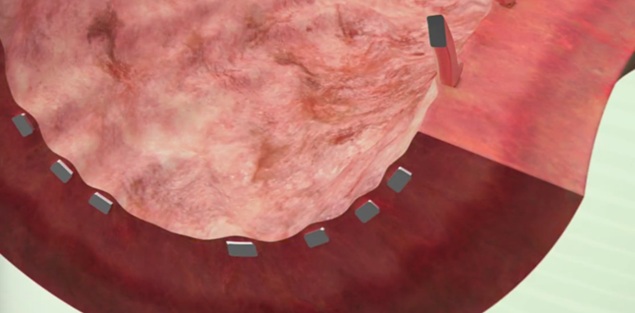
İlaçlı stent mi, ilaçsız stent mi daha iyidir? En iyi stent hangisidir?
In almost all cases, drug eluting stents are better than non-drug eluting stents. Hastanın klinik durumu ve damar yapısına göre değişmekle beraber ortalama olarak; ilaçsız stentlerde her 100 kişiden 15’inde, ilaçlı stentlerde ise 5’inde aşırı doku büyümesine bağlı stent içi darlık (ISR: Instent restenosis – Stent içi restenoz) gelişir. Ancak, aynı bilgiyi tersten okursak; ilaçsız stentlerde her 100 kişiden 85’inde, ilaçlı stentlerde ise 95’inde sorun gelişmez. Günümüzde, ilaçsız stentler no more is almost never preferred. At least, I myself (Dr. Şükrü Akyüz) have not used it for years.
Medicated stents have also improved considerably with technology. The latest generation of drug eluting stents is better than the previous generation. However, "better" does not mean "there is a huge difference between them". For example, while the probability of re-stenosis in the latest quality stent is %3 (3 out of every 100 people), this rate is around %5 in the previous generation of the same brand. As you can see, there is a difference, but it is not as marked as the difference between drug eluting and non-medicated stents.
What is a European stent?
Günlük hayatta hastalar arasında “Avrupa stent” ifadesi sık kullanılsa da aslında bu yanlış bir ifadedir. Kastedilen, ilaçlı stenttir. İlaçlı stentler sadece Avrupa’da üretilmezler; başta ABD olmak üzere pek çok ülkede üretilirler. Türkiye’de üretilen ilaçlı stent markaları da bulunmaktadır.
What is a dissolving stent?
Bir stentin zamanla eriyip kaybolması akla mantıklı gelse de son yapılan bilimsel araştırmalarda eriyen stentlerin metal olanlara göre hastaya ilave fayda sağlamadığı kanıtlandı. Hatta, bazı kısımlarının yeterince erimeyip damar içinde pıhtılaşmaya neden olduğu için bu stentlerin daha riskli olduğu anlaşıldı. Bu nedenle, eriyen stentler şimdilik tüm dünyada piyasadan kaldırıldılar. İyileştirmeler sonrası daha iyileri üretilene kadar bu stentlerin kullanımı artık şu anda söz konusu değildir.
“Eriyen” stentleri, “polimerleri eriyen stentler” ile karıştırmamak gerekir. Eriyen stentler tamamen eriyen stentlerdir. PIn the case of dissolvable stents, the only part that melts is the drug-carrying polymer embedded in the metal surface; the metal scaffold remains unmelted. PStents with dissolvable polymers are currently in use. However, the most important point that determines the quality of a stent is the clinical results obtained in comparative quality scientific studies rather than whether the stent is polymerized or not.
What is a medicated balloon?
Damar açmakta kullanılan balonlar, dış yüzeyi özel bir ilaçla kaplıysa “ilaçlı balon (DCB)” olarak adlandırılırlar. Bu ilaçlar balon şişirildiğinde damar duvarına nüfuz ederek aşırı doku büyümesini engellerler. Geniş, ana damarlarda ilaçlı stentler kadar etkili ve güvenli olduklarına dair henüz elimizde yeterli bilimsel veri bulunmamaktadır. Bu nedenle, günümüzde genellikle ince çaplı damar tıkanıklıklarında tercih edilirler. Bu balonlar hakkında daha detaylı bilgi için “Medicated Balloon” adlı sayfamızı ziyaret edebilirsiniz.
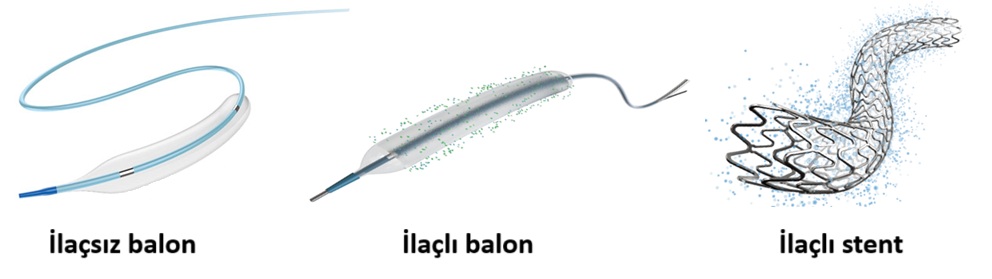
El bileğinden mi, kasıktan mı stent takmak daha iyidir?
Çoğu hastaya hem el bileği yoluyla hem de kasık yoluyla stent takılabilir. Ayrıntılar aşağıdaki gibidir:
- The most common complication of stenting is bleeding at the site of vascular access. This occurs less frequently at the wrist access site than in the groin and is less likely to be serious. Even if it does occur, it can be easily controlled by applying pressure by hand.
- The wrist is more comfortable for the patient than the leg. The inguinal route is more comfortable for the doctor.
- There is no need to lie on your back for 8-12 hours after the procedure in the wrist pathway. In fact, if the inguinal vein access site is closed with special inguinal closure devices rather than by pressing by hand, there is no need to lie on the back for a long time in the inguinal route.
- Since the wrist vein has a thinner diameter, it is much more likely to become blocked than the inguinal vein; blockage occurs in 1 in 10 patients. However, because there is an additional (backup) vein in the wrist, even if the wrist vein is blocked by a clot, the backup vein does not cause any problems; in fact, it is extremely rare. The groin vein is less likely to become blocked, but because it is the only vein leading to the leg, if it does become blocked, emergency stenting or surgery may be required.
- The wrist vein is more prone to catheter-induced spasm (constriction). The spasm can cause the vein to compress the catheter, which in some patients can cause difficulty in retracting the catheter and severe pain.
- Infection is much less likely to develop at the wrist vein entry site than in the groin. If infection develops in the groin, it can sometimes have very serious consequences.
- Not all procedures and not all patients are technically suitable for wrist procedures. Both the anatomy of the wrist must be appropriate (e.g. the wrist vein must not be too thin or tortuous) and the doctor must be experienced in wrist procedures.
- In some patients, for clinical and anatomical reasons, it may be necessary to use the inguinal route or the wrist route.
- Whether it is the inguinal route or the wrist route, the procedure applied to the heart is the same.
Sonuç olarak, mümkünse el bileği tercih edilmelidir. El bileğinin tercih edilmesine dair önerinin en önemli nedeni, en sık görülen komplikasyon olan kanamanın kasık yoluna göre daha az sıklıkta ve ciddiyette olmasıdır. Ancak, yukarıda bahsettiğimiz detaylar nedeniyle nihai kararı işlemi yapacak olan hekime bırakmak en doğrusudur.
What should be considered after a stent procedure?
You should inform your doctor if the following happens at the site of the procedure (groin or wrist)
- Bleeding (in such a case, you should press the bleeding area with your hand and call 112)
- Giderek büyüyen şişlik (Fındık büyüklüğünü geçmeyen şişlik normaldir)
- Giderek artan kızarıklık (Hafifçe kızarıklık, şişlik, morluk veya hassasiyet olması normaldir)
- İltihaplı akıntı (Ara ara az miktarda şeffaf akıntı normaldir)
- Aşırı ağrı (Ağrınız zamanla azalıyorsa, bu normaldir)
- Numbness in the leg or wrist that does not go away
- Fire
- If your symptoms before stenting, such as chest pain or shortness of breath, recur a few minutes rest or take sublingual medication. If your chest pain does not go away despite rest or sublingual medication, go to the nearest emergency room or call 112.
- Stop smoking; don't just cut down.
- Don't drink alcohol; at least cut down (It used to be thought that drinking small amounts of alcohol, especially wine, could be good for the heart. However, new scientific evidence suggests that it is probably best not to drink alcohol at all. This is the recommendation of the latest European Society of Cardiology "Guidelines for the Prevention of Cardiovascular Disease").
- Do not gain weight; if you are overweight, reduce your weight with a healthy diet and exercise program.
- Keep your cholesterol levels under control (by watching what you eat and taking medication).
- Keep diabetes and hypertension under control.
- Exercise regularly; at the very least, avoid elevators, driving everywhere and sitting all the time.
- Take your heart medicines (especially blood thinners) regularly.
- Watch what you eat (more details below).

How should the patient with a stent be fed?
Recommended by international guidelines Mediterranean style Remember that this way of eating applies to everyone, whether they have cardiovascular problems or not. The difference in the patient with a stent is that tighter to comply with the law (See. References).
- Eat a diet based on vegetables and fruits. Make sure they are fresh and in season.
- Eat more nuts such as walnuts, hazelnuts and almonds (unsalted and raw), fish, legumes (dried beans, kidney beans, chickpeas, lentils) and fiber.
- Don't eat too much bread. But, ever It is not right not to eat bread. Choose whole wheat bread instead of white bread.
- Cut down on sweets and sugary drinks (cola, soda, fruit juices, etc.); if possible, eliminate them from your life. Ask for water or mineral water with your meals.
- Avoid processed meats (sausages, pepperoni, salami, etc.). In fact, avoid everything processed.
- Use less salt; no more than 5 grams per day.
- Avoid snacks such as fast food, chips and biscuits.
- Choose low-fat or fat-free dairy products.
- Avoid trans fats such as margarine. Cook with healthier fats such as olive oil or sunflower oil.
- Do not consume too much animal fats (saturated fats) such as butter. In fact, with the new data, this issue has become somewhat controversial. Namely, ever It is probably not right not to consume it. For example, you can eat butter for breakfast. It is also okay to eat eggs.
- You can eat up to 500 grams of lean red meat per week. However, we do not recommend eating offal.
- You can also drink herbal teas, black tea and coffee twice a day, but too much can cause palpitations.
- Although a plant-based diet is generally considered to be healthier, do not be under the misconception that all plant foods are beneficial and all animal foods are harmful. For example, remember that white flour and refined sugar, which are known to be harmful, are plant foods, while fish, which is known to be beneficial, is an animal food.
- “Can veins be opened with herbal treatment?", which we recommend you also read.
Stent kalp krizini önler mi?
Stenting heart attack We now clearly know that stenting saves lives when it is performed in emergencies such as chest pain and shortness of breath. However, stenting is often performed in non-emergency situations, but only in chronic complaints such as chest pain and shortness of breath. In these cases, the main task of the stent is to relieve the symptoms. Stenting success in preventing heart attacks, scompared to the use of medication alone is actually similar in most cases. Exceptions are stenoses at the beginning of large arteries (for example, a stenosis in the so-called LMCA). In these cases, stenting is more successful in preventing heart attacks than using medication alone.
How long does a stent last? Can the stent get blocked?
Teknik açıdan başarılı olan bir stent işlemi sonrası hastanın; ilaçlarını düzenli kullanması, yüksek tansiyon ve diyabet gibi risk faktörlerini kontrol etmesi ve sağlıklı yaşam tarzını uygulamaya başlaması stentin daralma veya tıkanma olasılığını oldukça azaltır. In complex cases, there are usually problems in more places, so more stents are needed. The more and longer the stent, the more likely it is that excessive tissue growth will occur. in the stent darlık (in-stent restenoz) gelişme olasılığı da o kadar fazla olur (Damar çapının %100’üne ulaşan ve kan akımını tamamen engelleyen darlığa “tıkanıklık” adı verilir). However, this should not be interpreted to mean that the stents are likely to narrow. In 10 years stentte darlık gelişmesi; kompleks olmayan (olağan) her 10 vakanın sadece 1’inde while the complex one occurs in 2 out of 10 cases.
Tersten okunduğunda, kompleks olmayan vakaların %90’ında, kompleks vakaların ise %80’inde stentlerde darlık gelişmez. Darlık gelişecekse çoğu vakada ilk 1 yıl içinde olur. Ayrıca, For those who develop stenosis, a second procedure solves the problem in about half of the cases and stenosis does not develop again. Stentin pıhtıyla aniden tıkanıp kalp krizine yol açması ise her 100 kişiden sadece 1’inde görülen bir tablodur. Bunun pek çok nedeni olsa da en sık nedeni hastanın kan sulandırıcı ilaçlarını kullanmamasıdır. Özetle, stentlerin belli bir ömrü yoktur; çoğu hastada stentler ömür boyu açık kalırlar.
How is stent blockage treated?
Stent içi darlık ya da tıkanıklıkta ilk çözüm yolu, stentin içine tekrar bir stent or widen the stenosis with a medicated balloon. Possibility of re-narrowing bwith the intervention is considerably reduced. For patients who very rarely experience recurrent in-stent stenosis bypass surgery may be necessary.
How many years will a patient with a stent live?
Stentlerin belli bir ömrü yoktur. It is not possible to know exactly how many years the patient will live. Estimated percentages can only be given by looking at the statistics of previous patients with the same characteristics. The most important factors that negatively affect this statistic are the following: Technical inadequacy in the stenting procedure, holder age, heart failure, heart valve disease, the presence of serious diseases in other organs, hypertension, diabetes, high cholesterol, smoking, medication non-compliance and lack of social support.
Stent or bypass?
Kalp cerrahları ve girişimsel kardiyologlar, damarlardaki sorunları tedavi eden iki farklı doktor grubudur. Kalp cerrahları, damar sorunlarını ameliyatla (bypass) çözerlerken; girişimsel kardiyologlar aynı sorunları ameliyatsız yöntemlerle (kompleks stent işlemleri) çözerler. For this important issue “Stent or Bypass?“ named in detail our article and watch our case study videos on the same page.

Prof. Dr. Şükrü Akyüz is an interventional cardiologist. His professional interest is the treatment of heart diseases with non-surgical methods. This includes the non-surgical opening of complex vascular blockages with special stenting methods.
References
5. Libby P, Bonow RO, and Mann DL, eds. Braunwald’s heart disease: A textbook of cardiovascular medicine, 12th ed. Philadelphia PA: Elsevier; 2022.
6. Brilakis E. Manual of chronic total occlusion percutaneous coronary interventions: A step-by-step approach, 3rd ed. Philadelphia PA: Elsevier; 2023.
7. Brilakis E. Manual of percutaneous coronary interventions: A step-by-step approach, 1st ed. Philadelphia PA: Elsevier; 2021.

